Overview
- Tubular organ extending from the pylorus of the stomach to the ileocecal valve.
- Average length in adults is 6-7 m.
- Composed of 3 segments:
- Duodenum: The shortest and most proximal segment, extending from the pylorus to the duodenojejunal flexure. It receives bile and pancreatic secretions and plays an important role in chemical digestion.
- Jejunum: The middle segment, specialized for nutrient absorption. It has no sharp anatomic boundary with the ileum.
- Ileum: The most distal segment, ending at the ileocecal valve. Particularly important for the absorption of bile salts and vitamin B12.
- Functions:
- Digestion of chyme by pancreatic enzymes and bile, and absorption of nutrients.
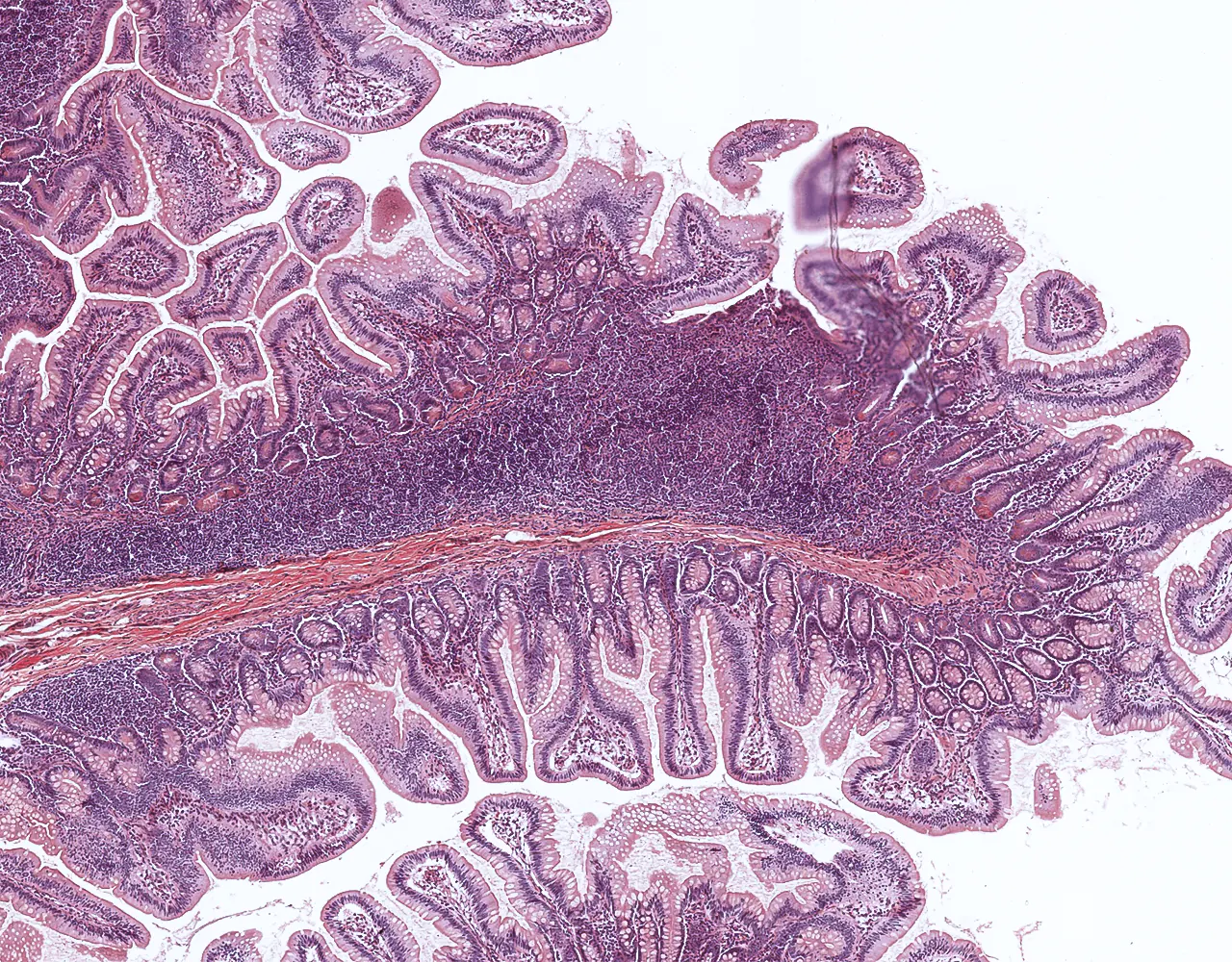
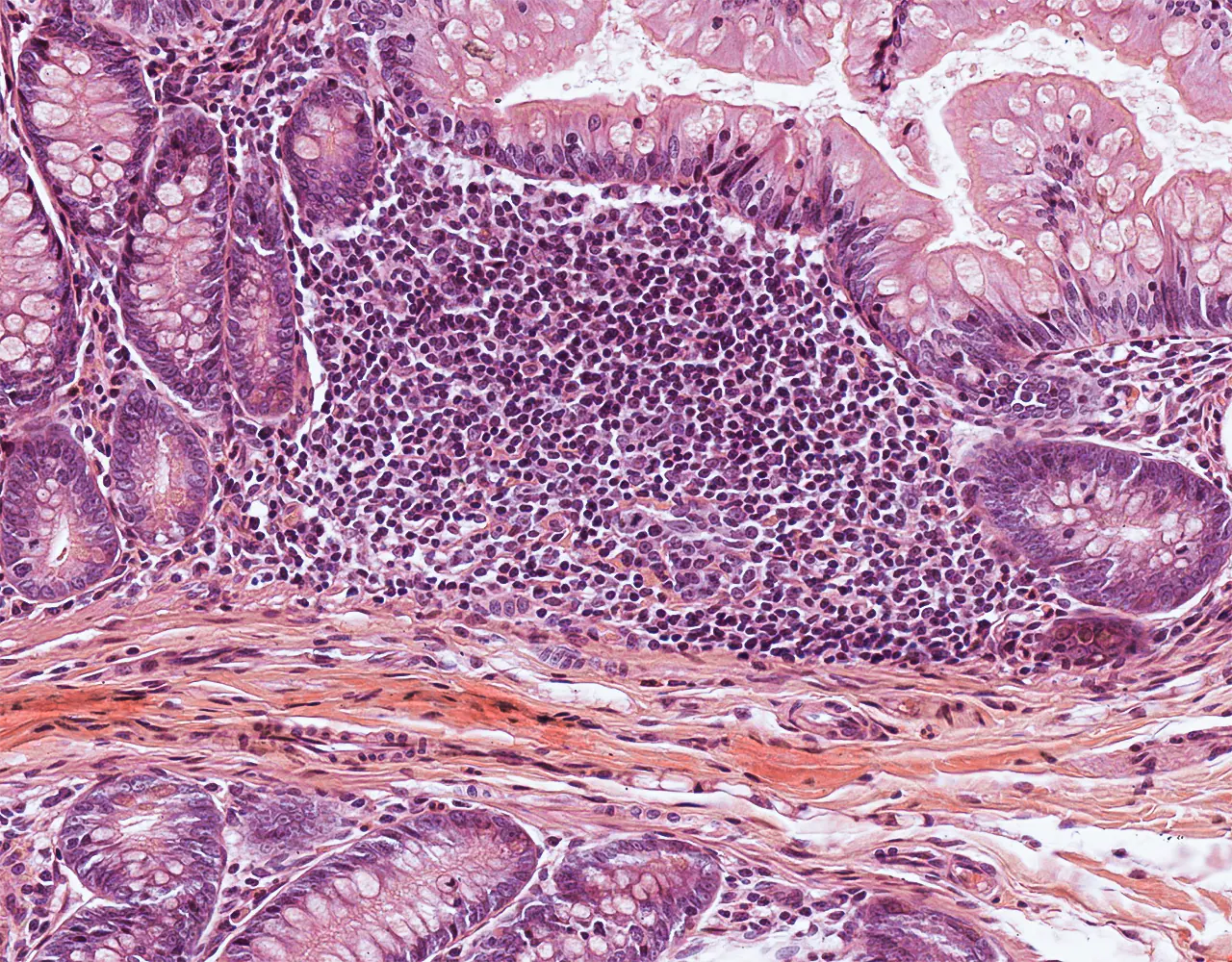
- Contribution to immune defence through gut-associated lymphoid tissue, especially Peyer patches in the ileum.
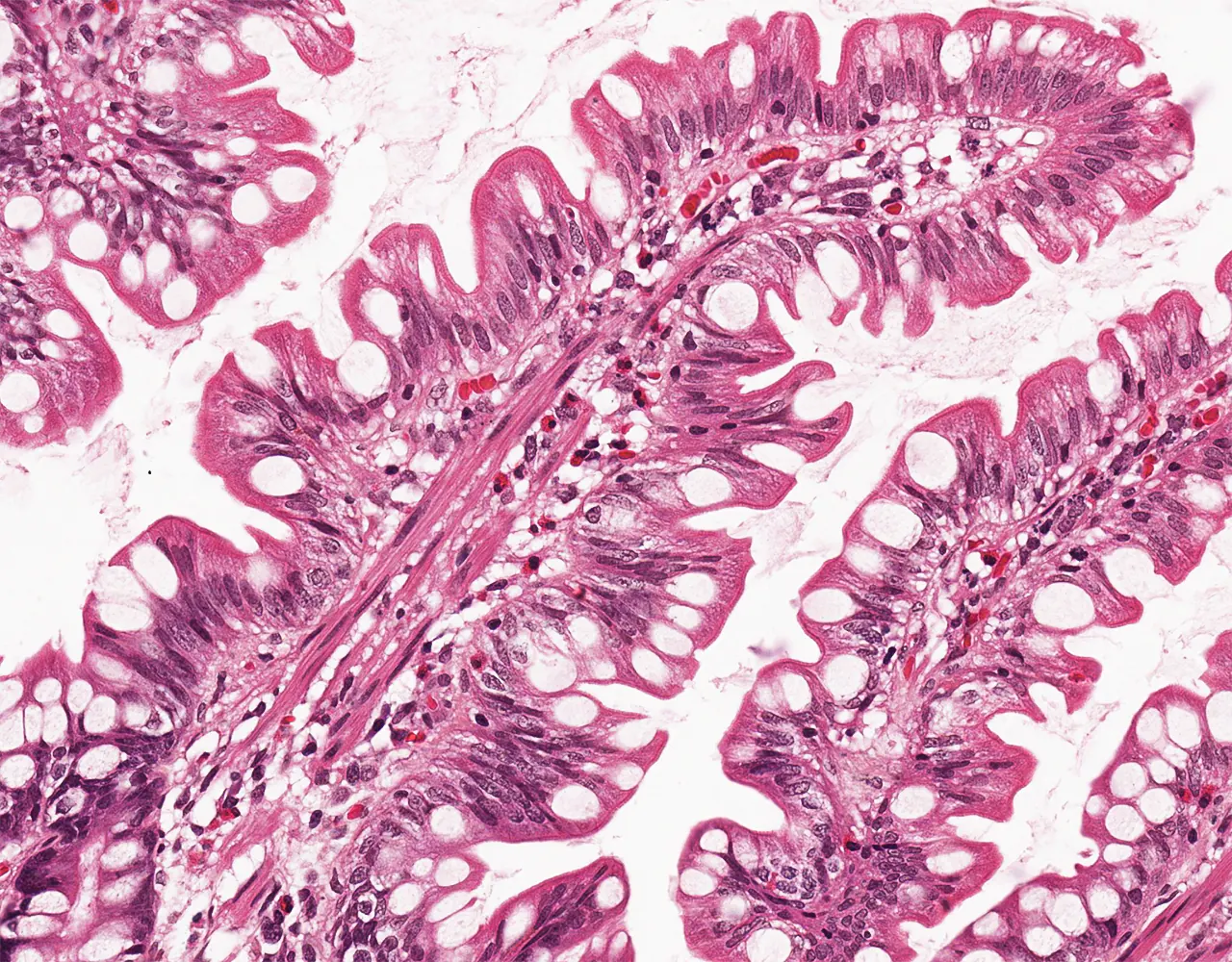
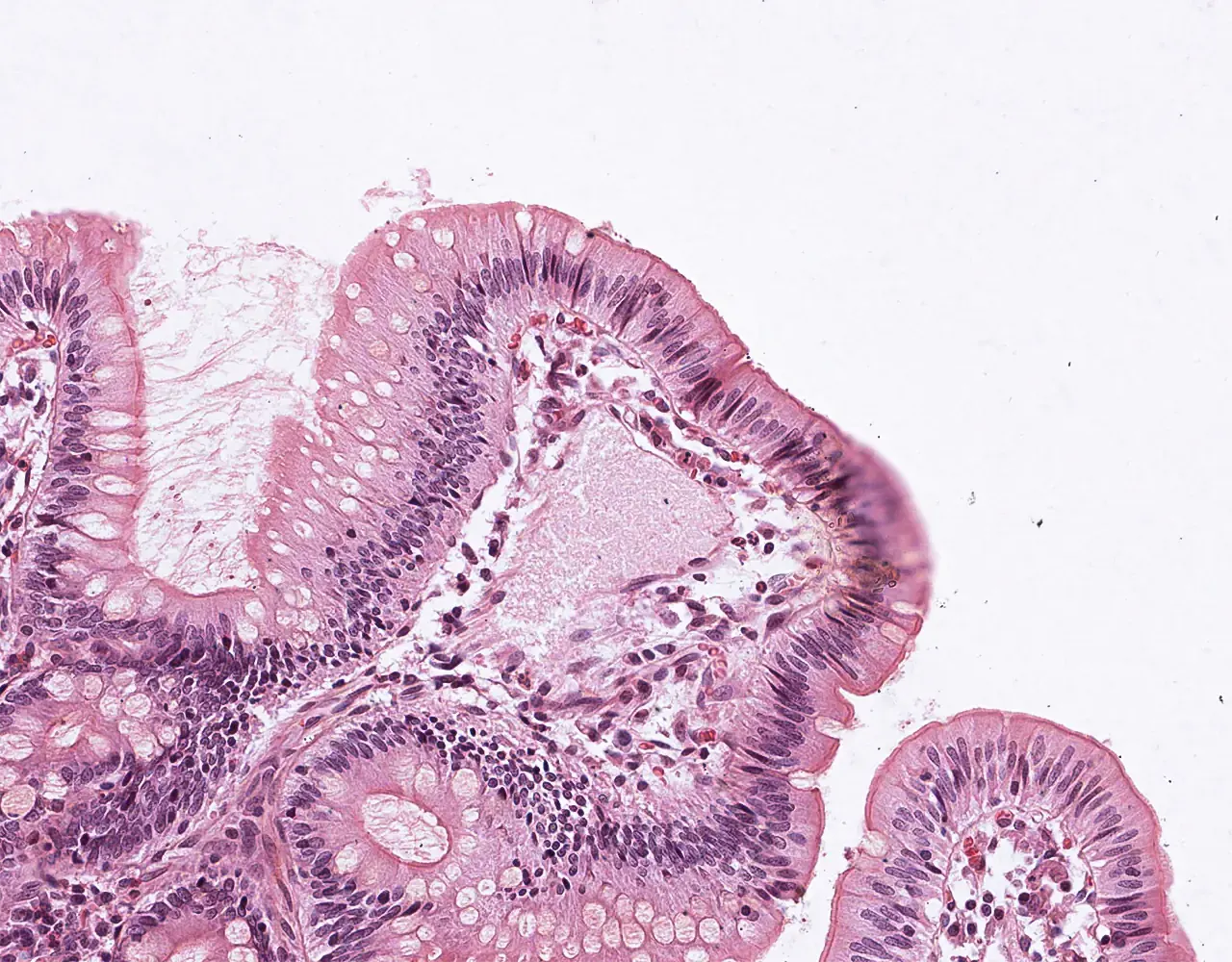
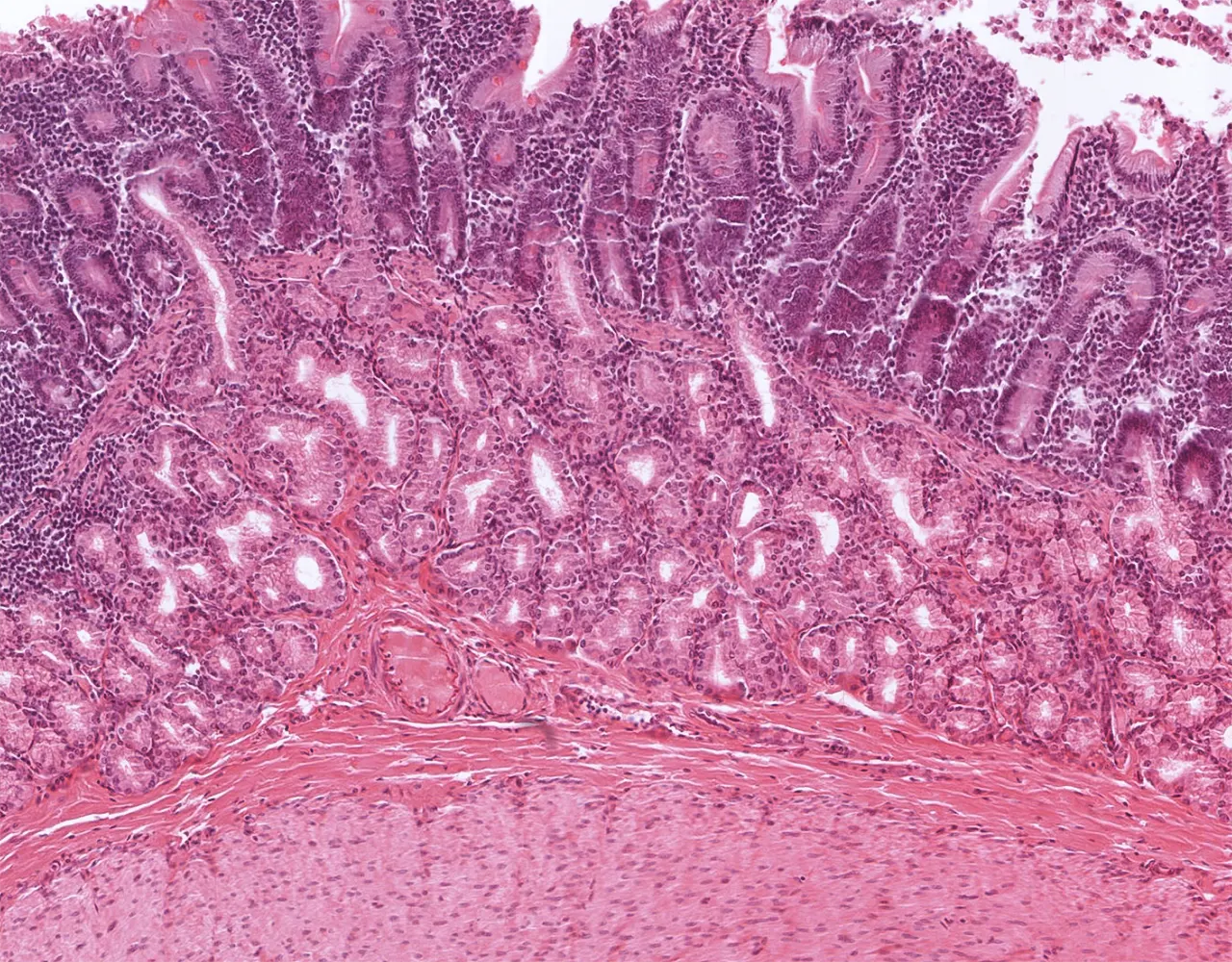
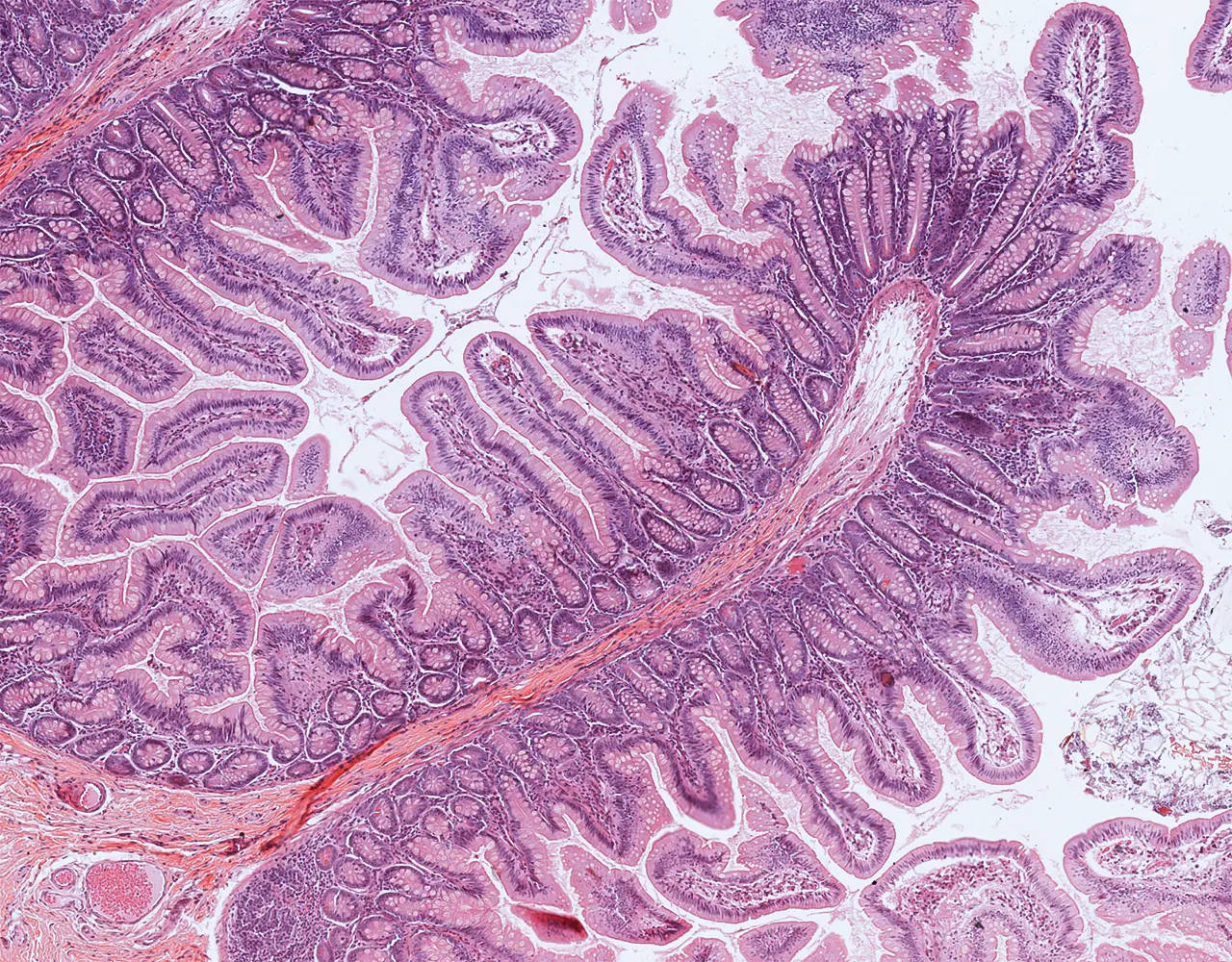
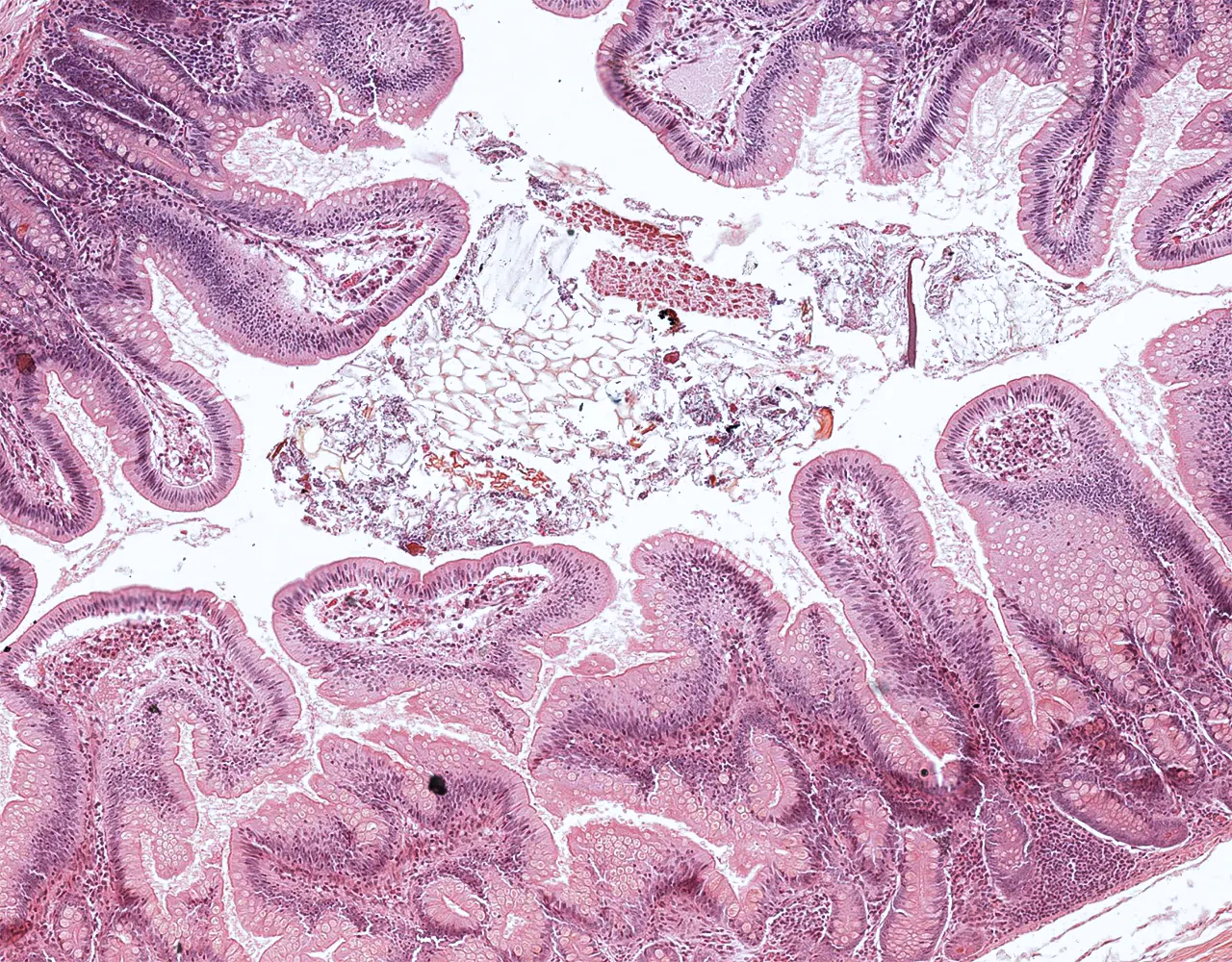
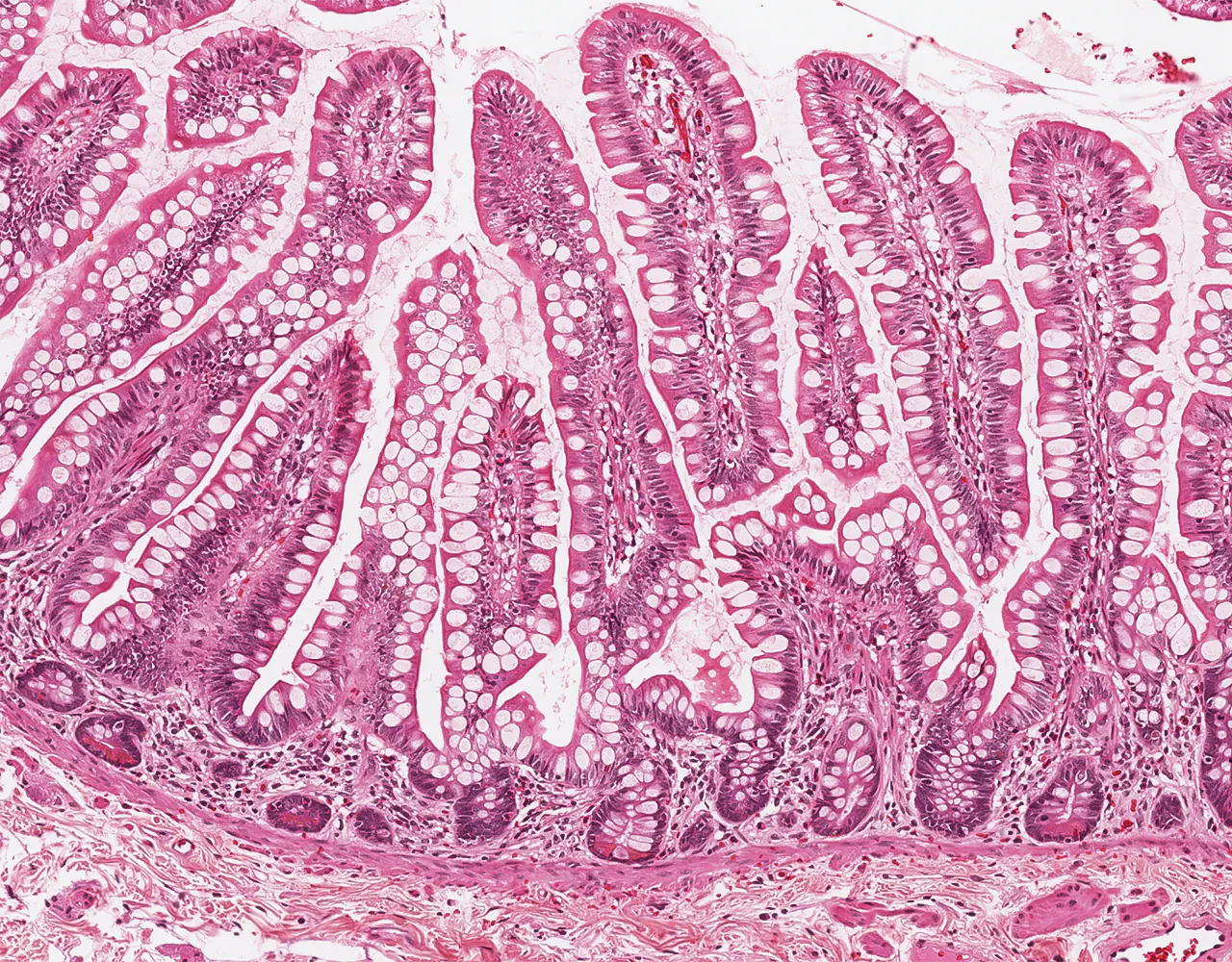
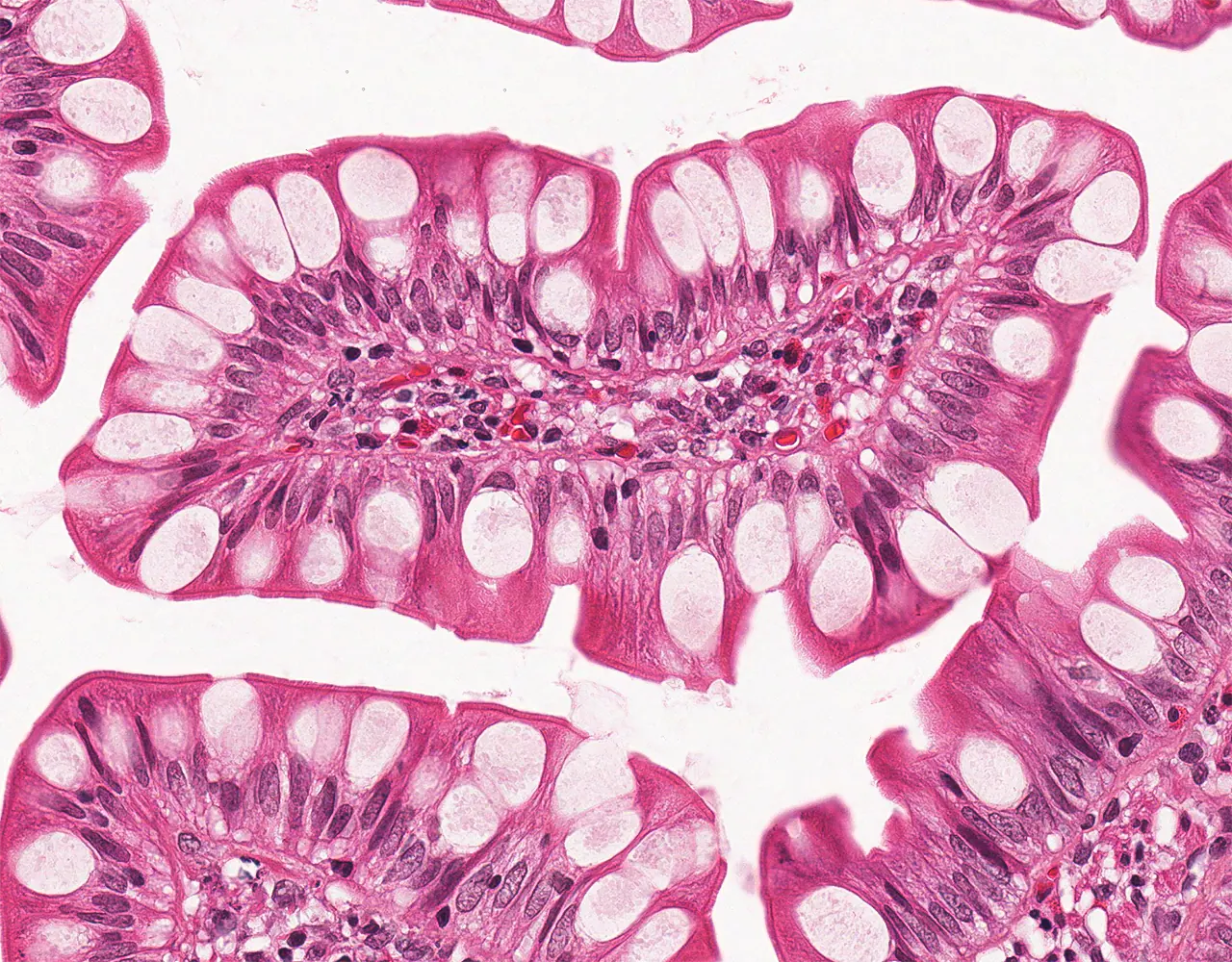
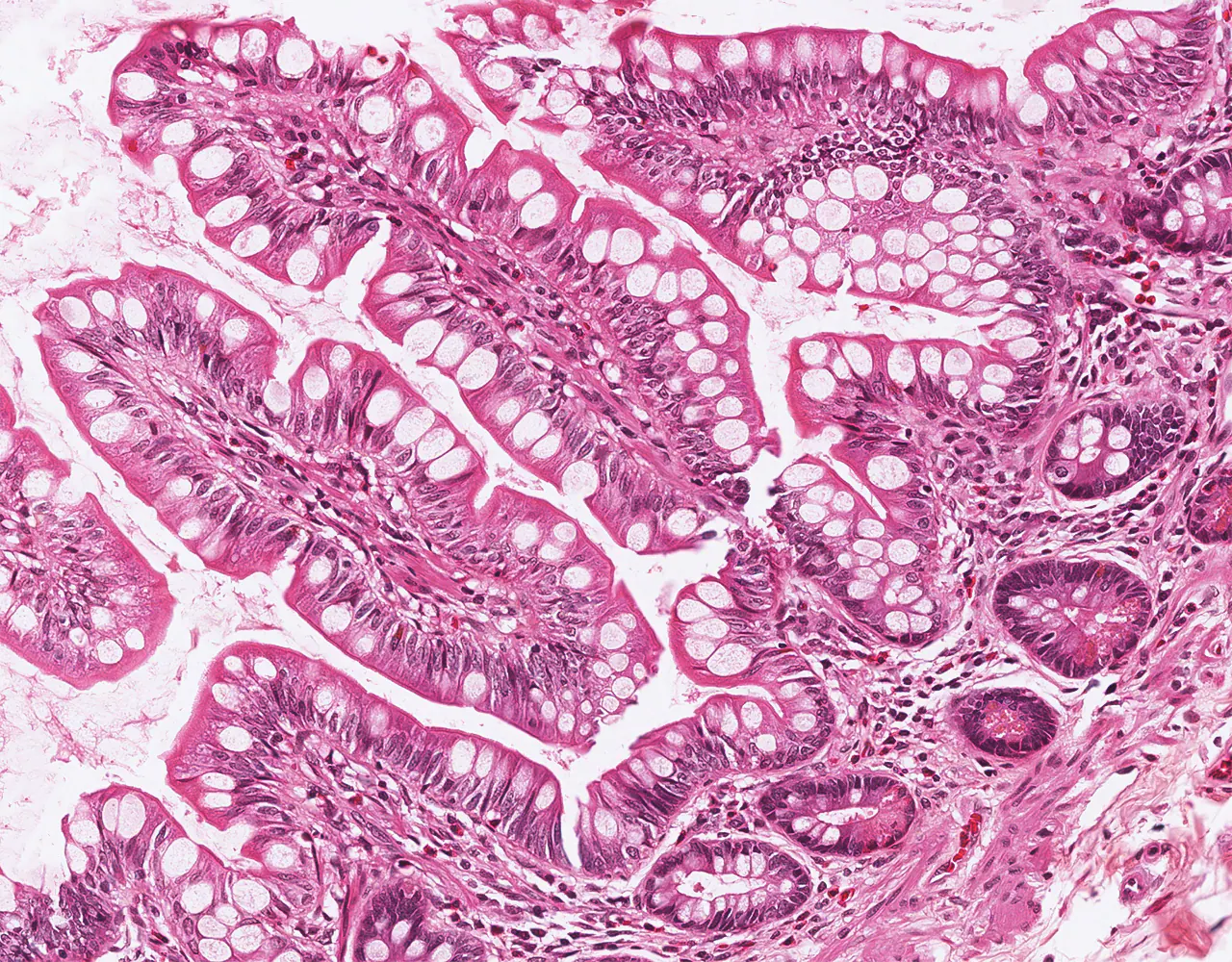
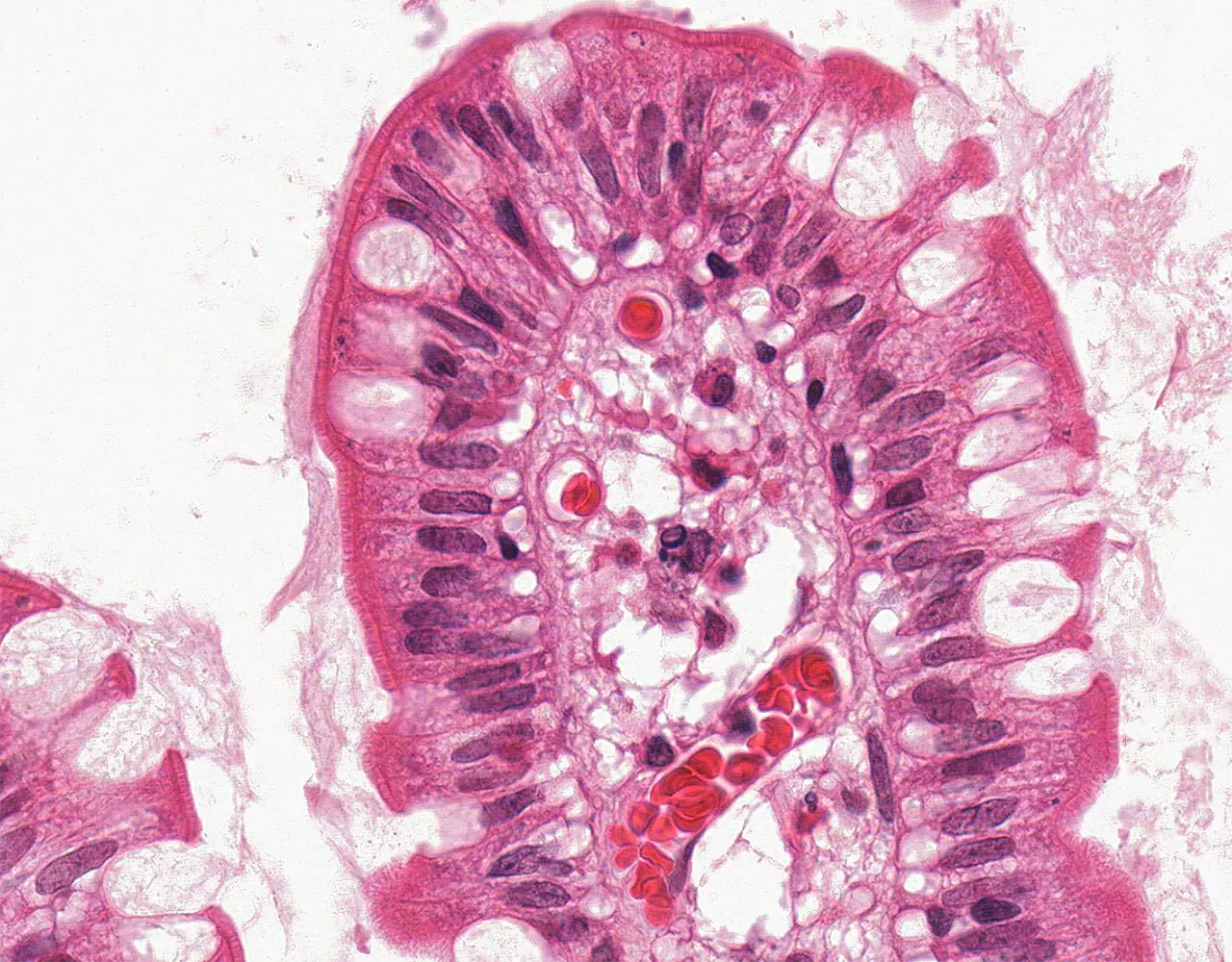
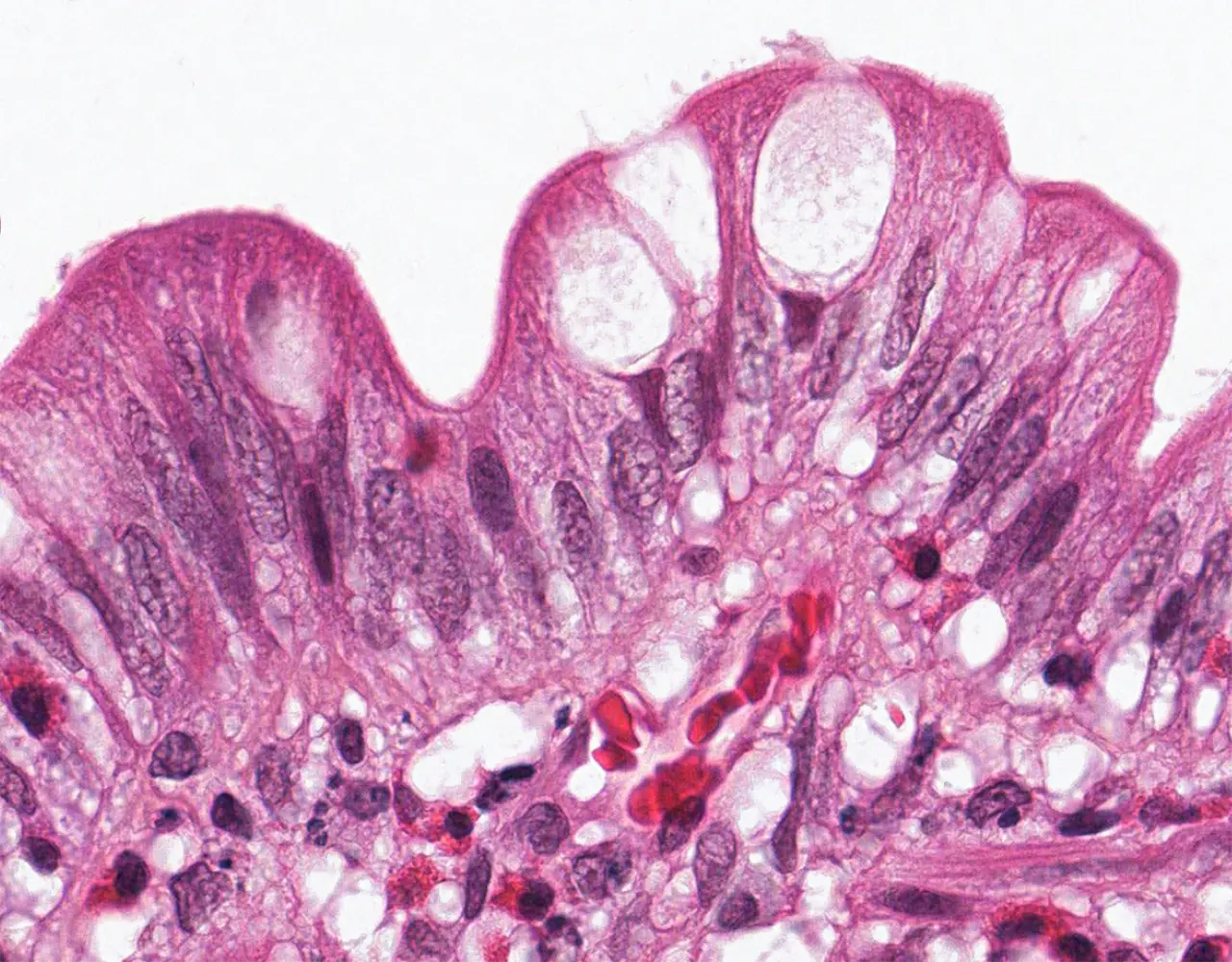
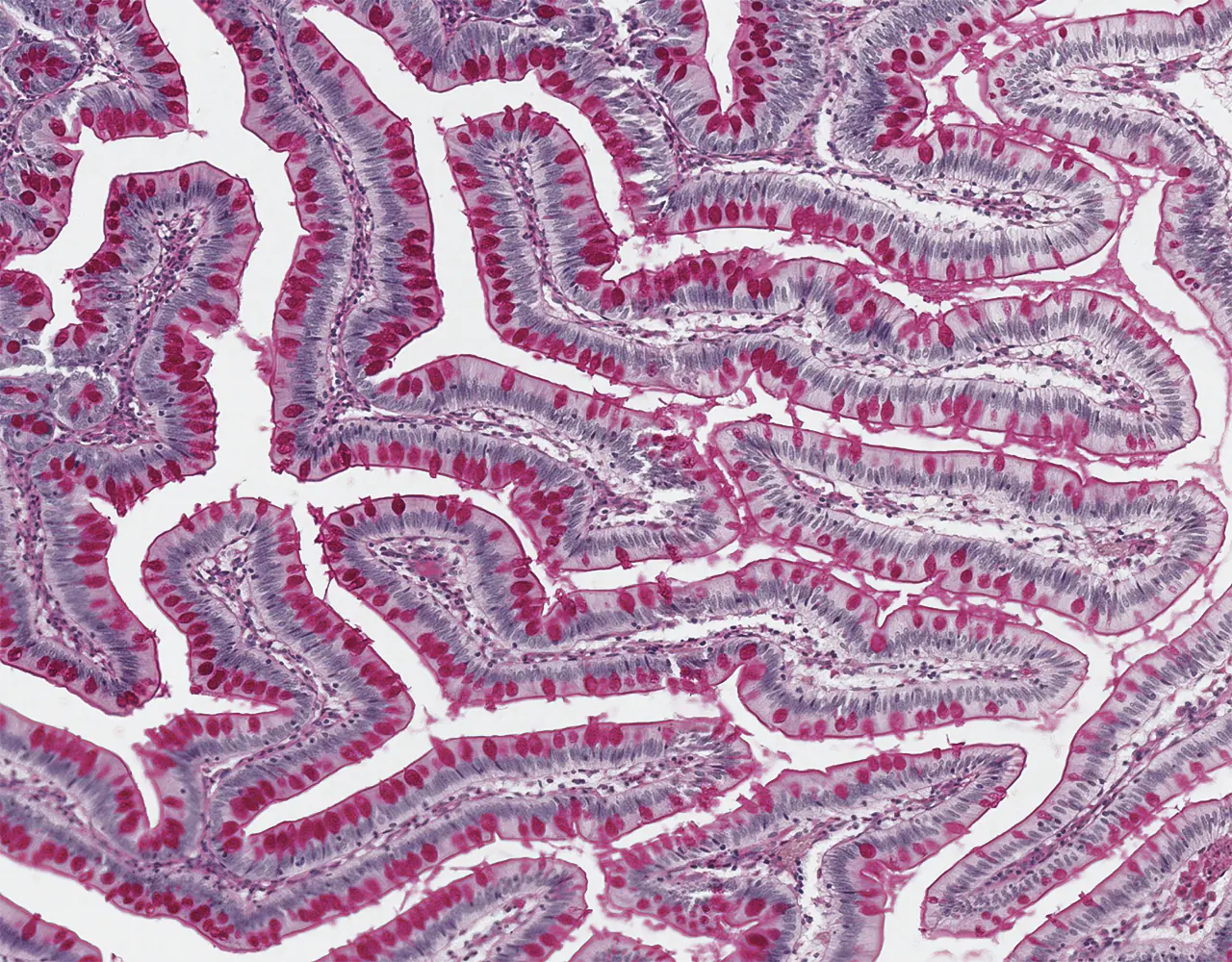
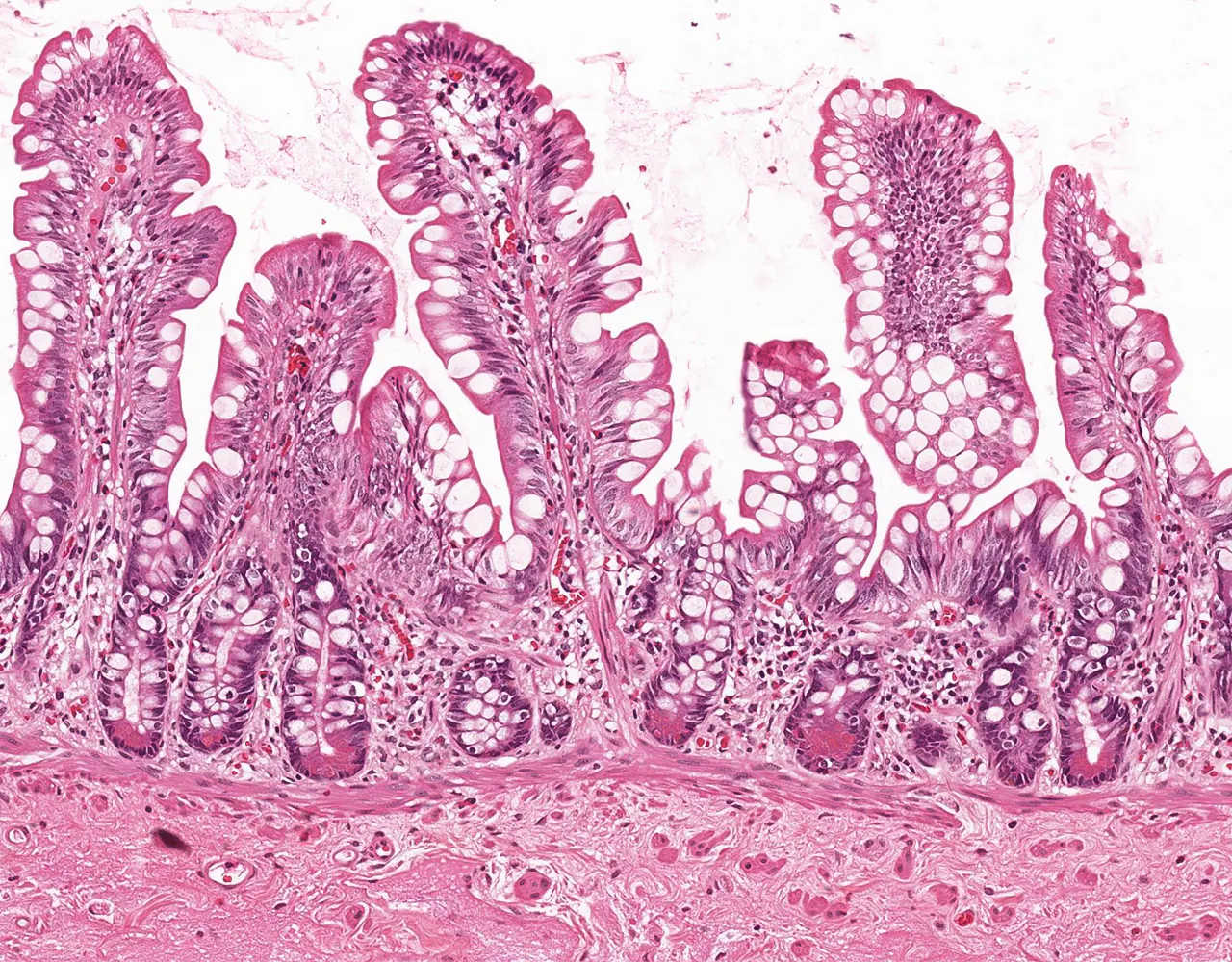
- The absorptive surface area of the small intestine is amplified by three structural levels: plicae circulares, villi, and apical microvilli forming the brush border.
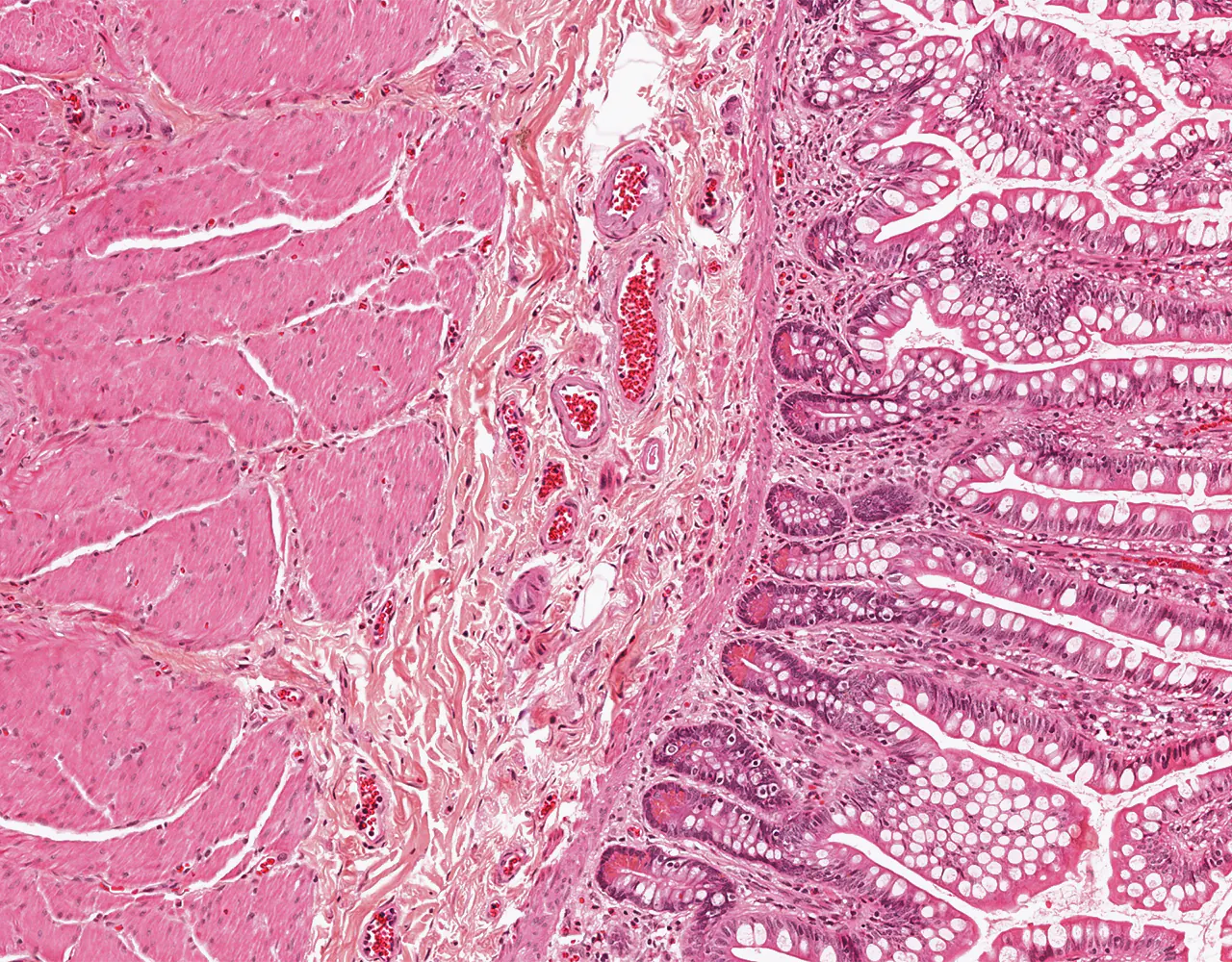
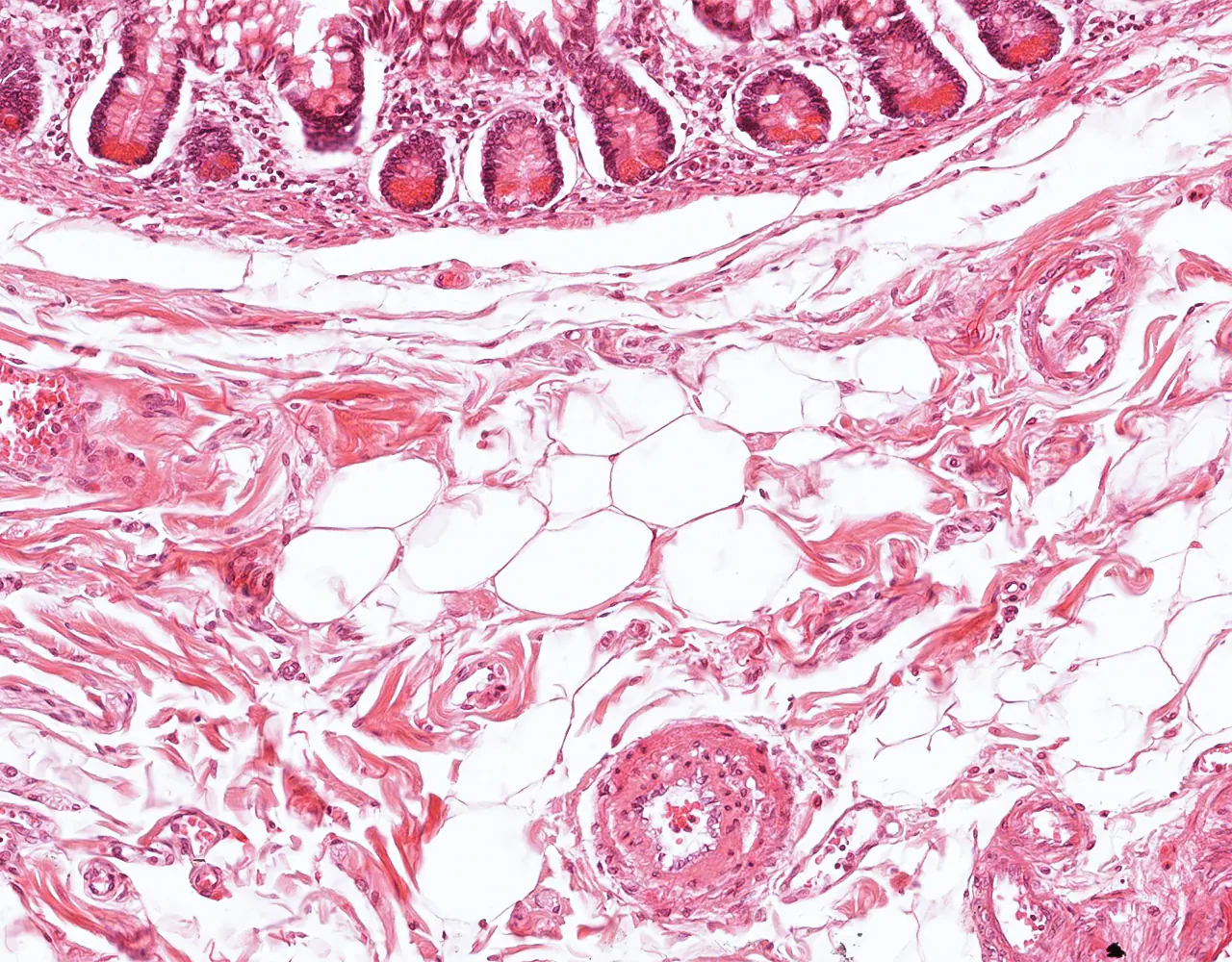
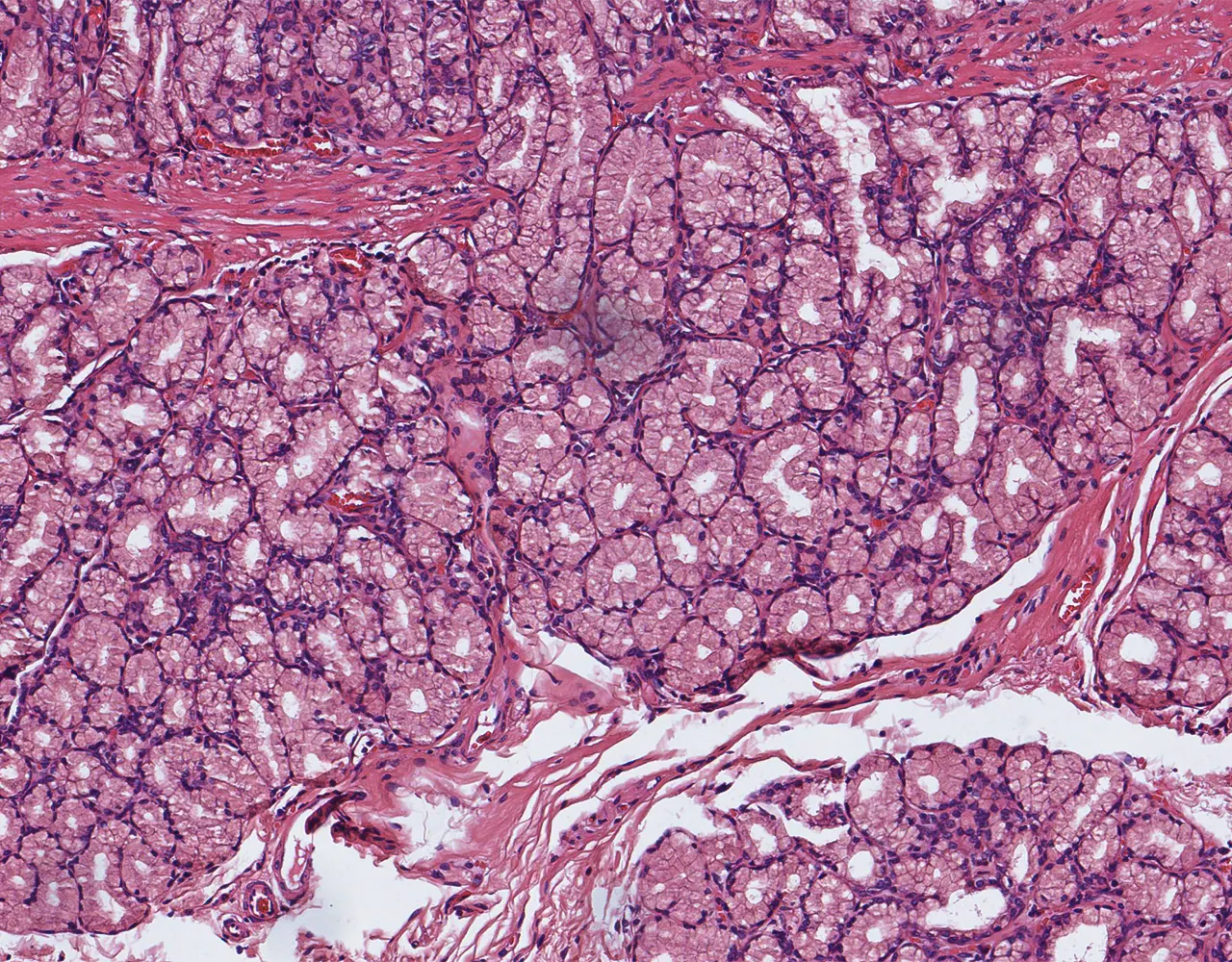
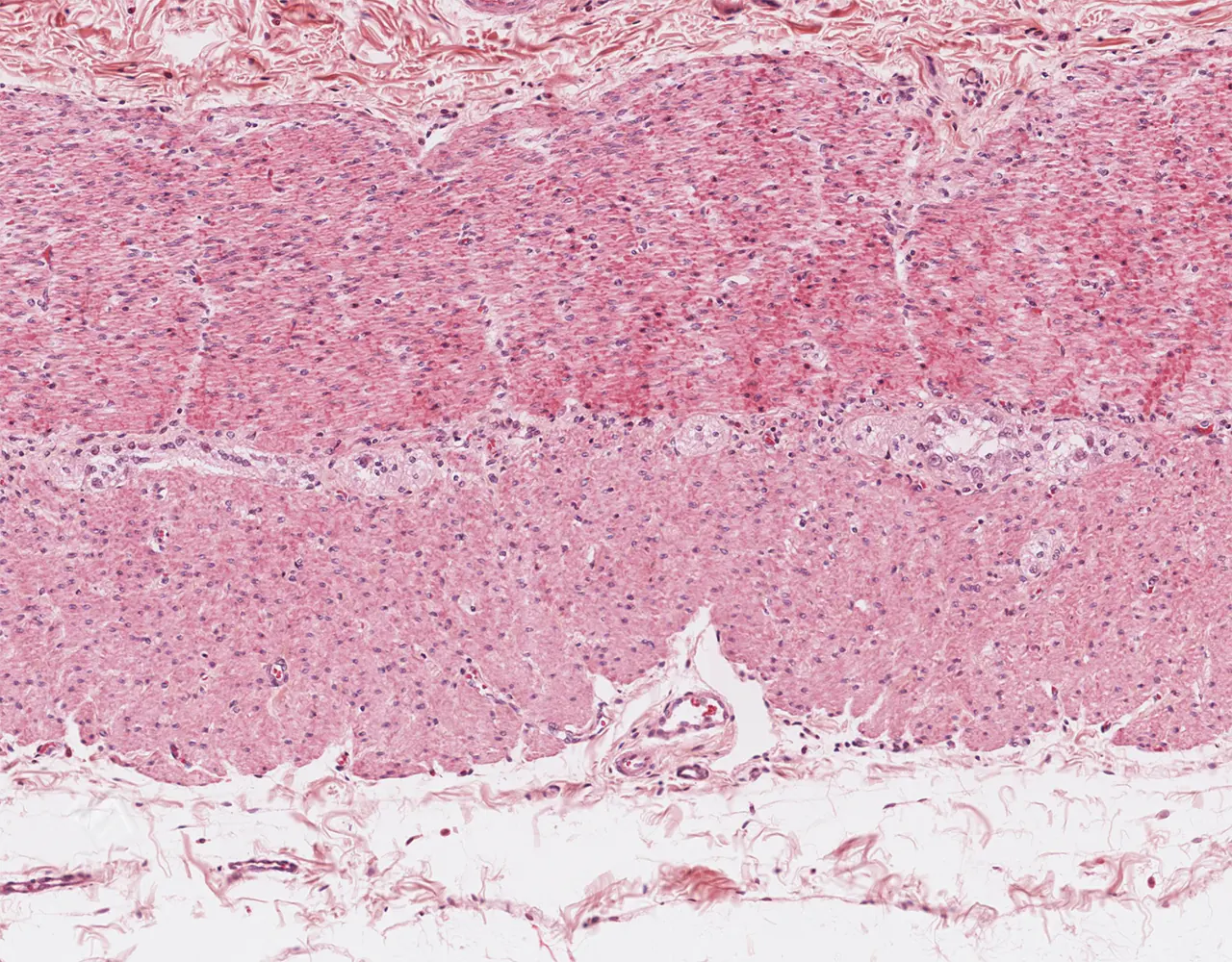
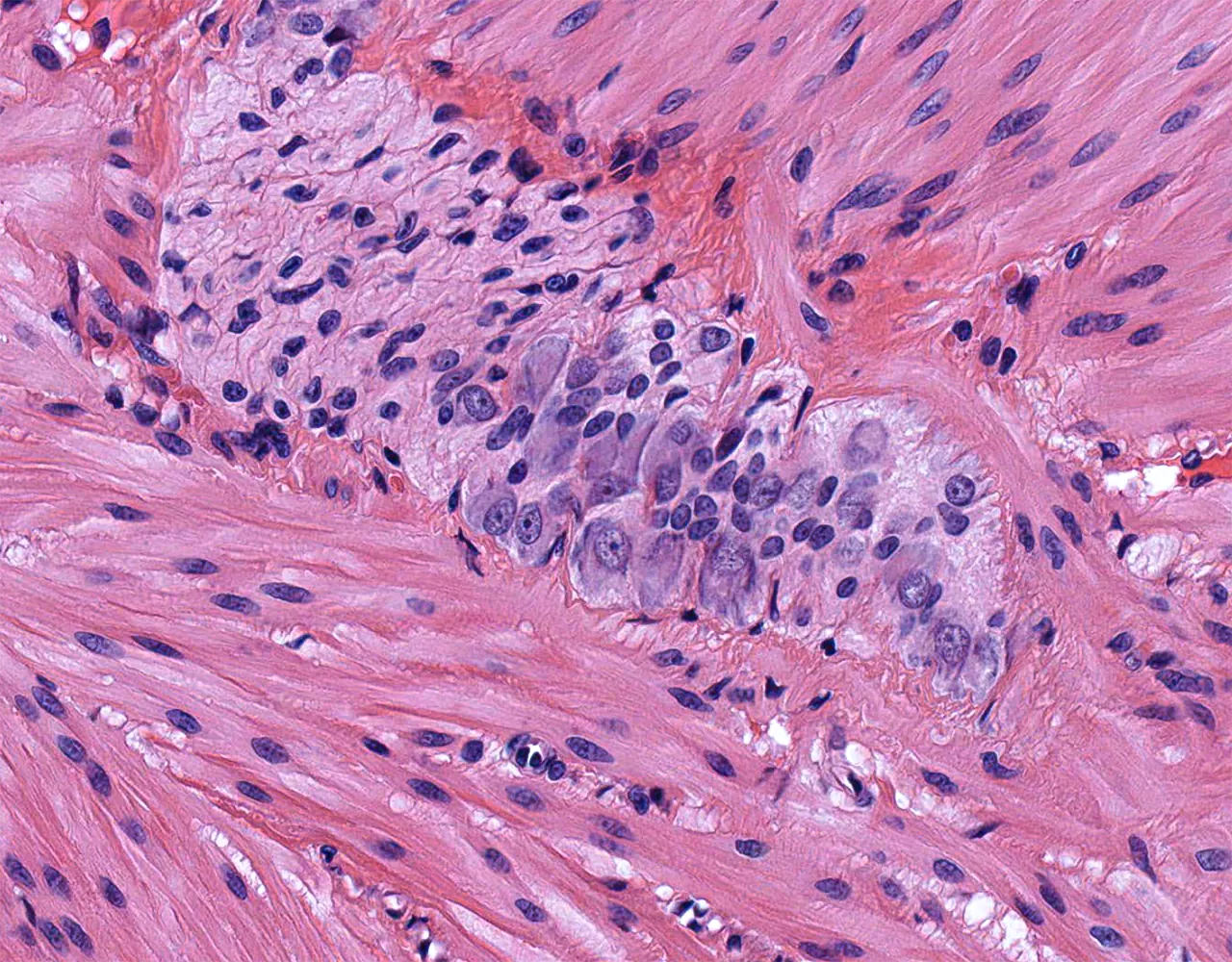
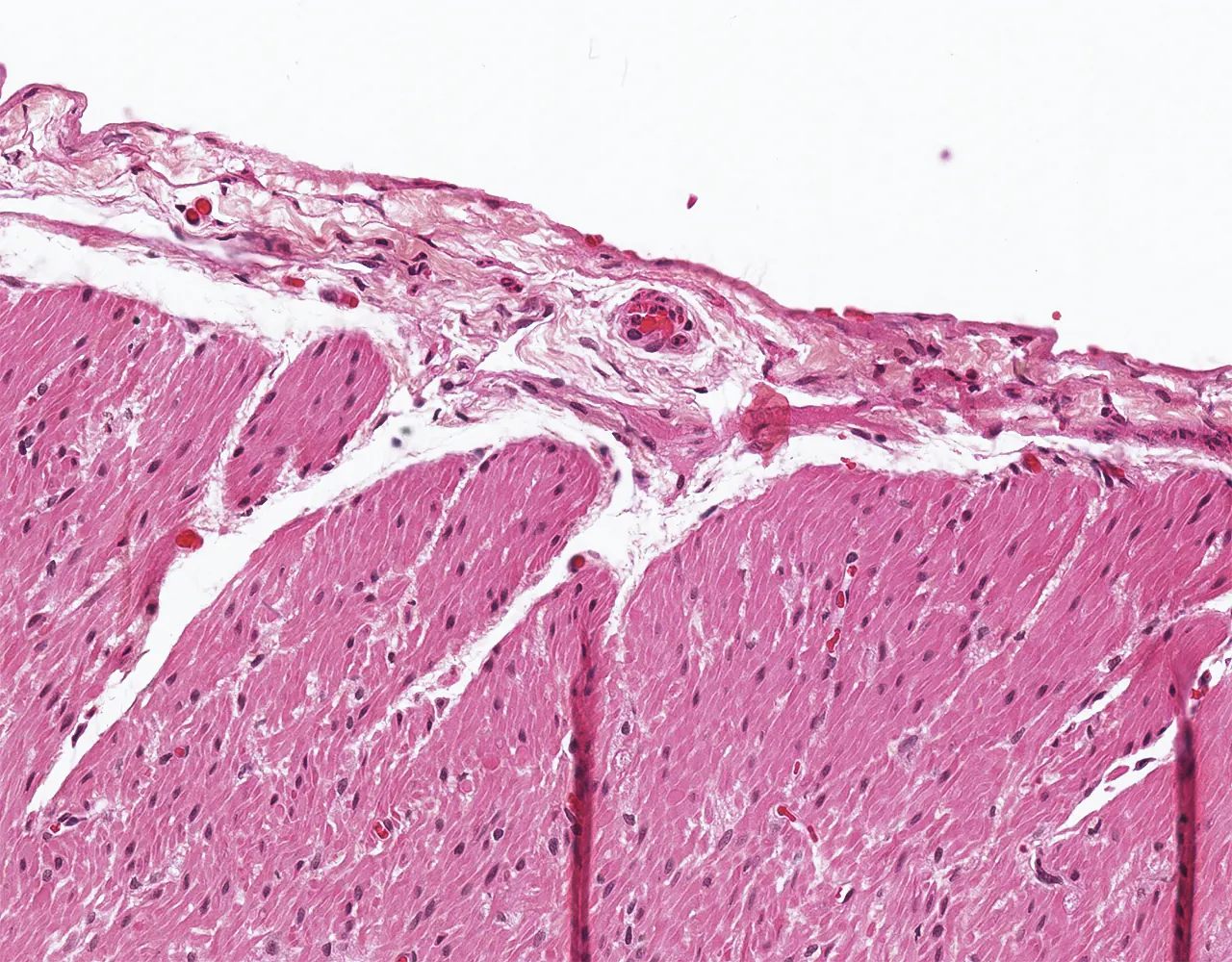
- Microscopically, the wall is composed of 4 layers from the inside outward: mucosa, submucosa, muscularis propria, and serosa.

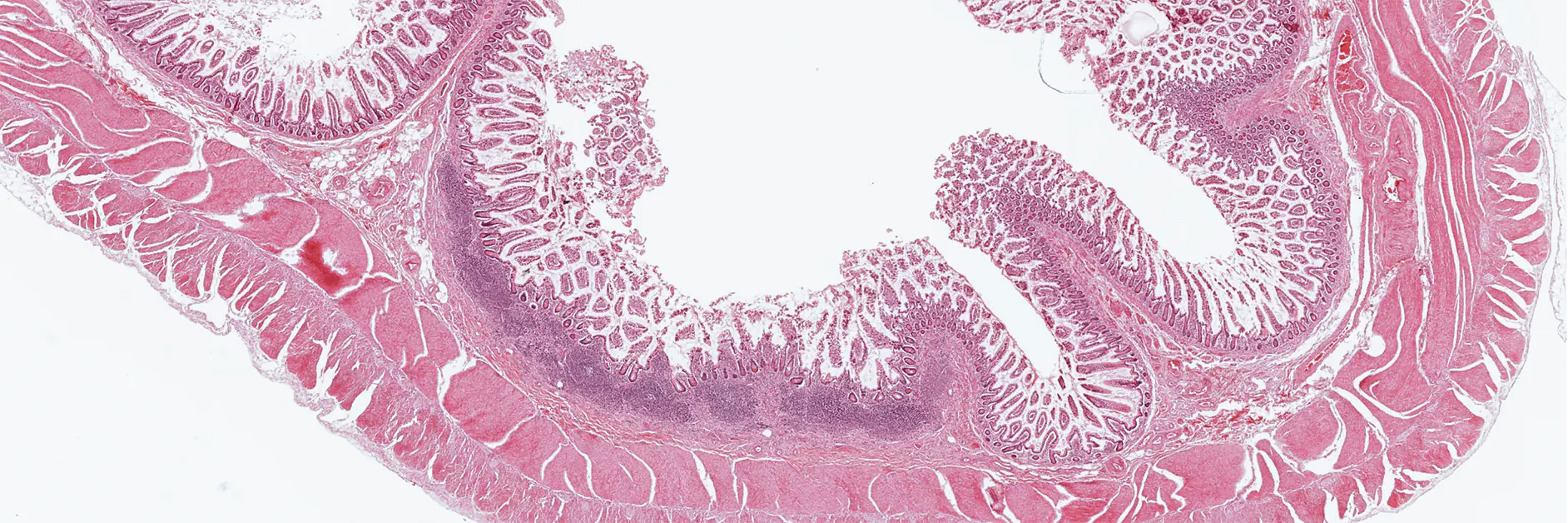
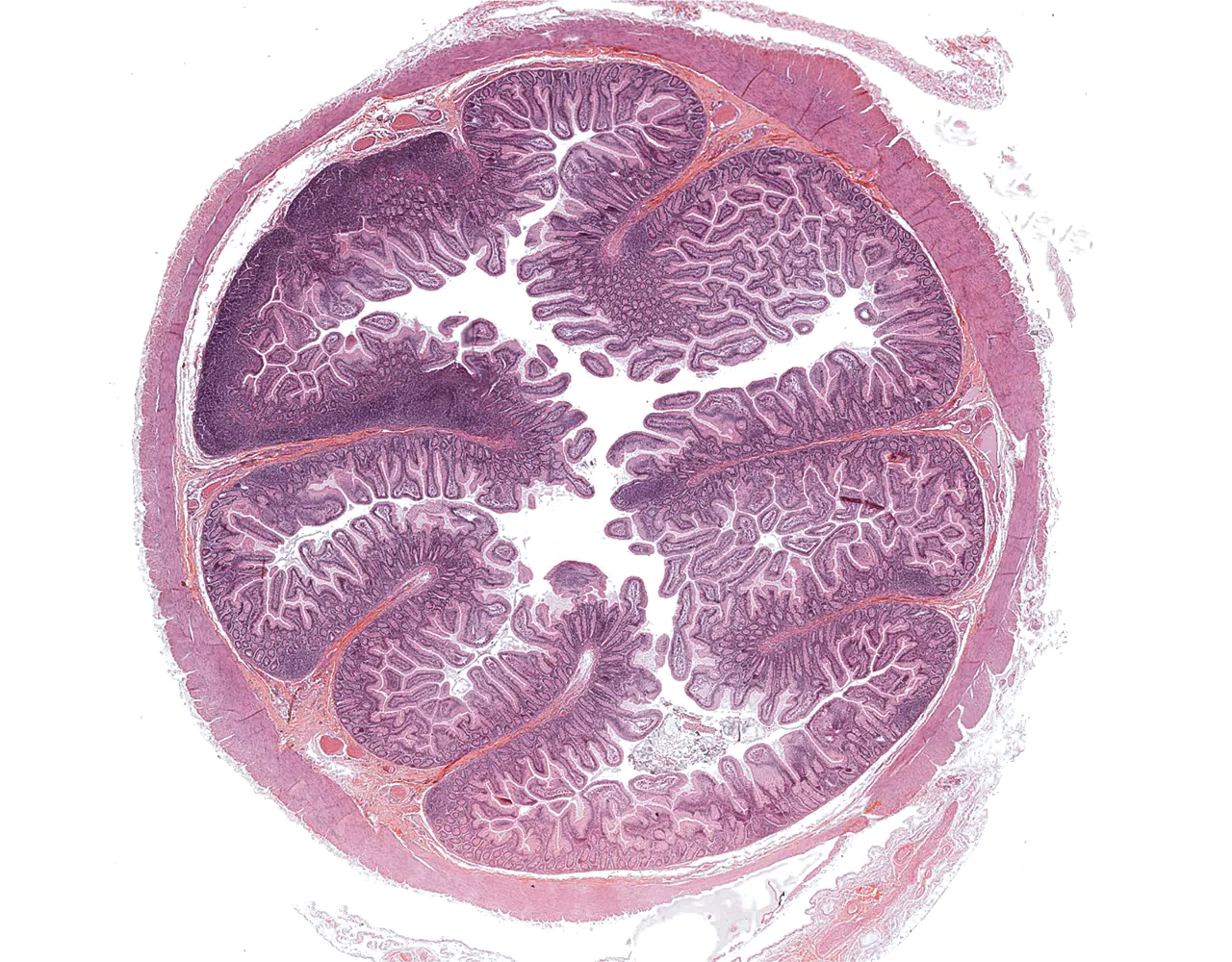

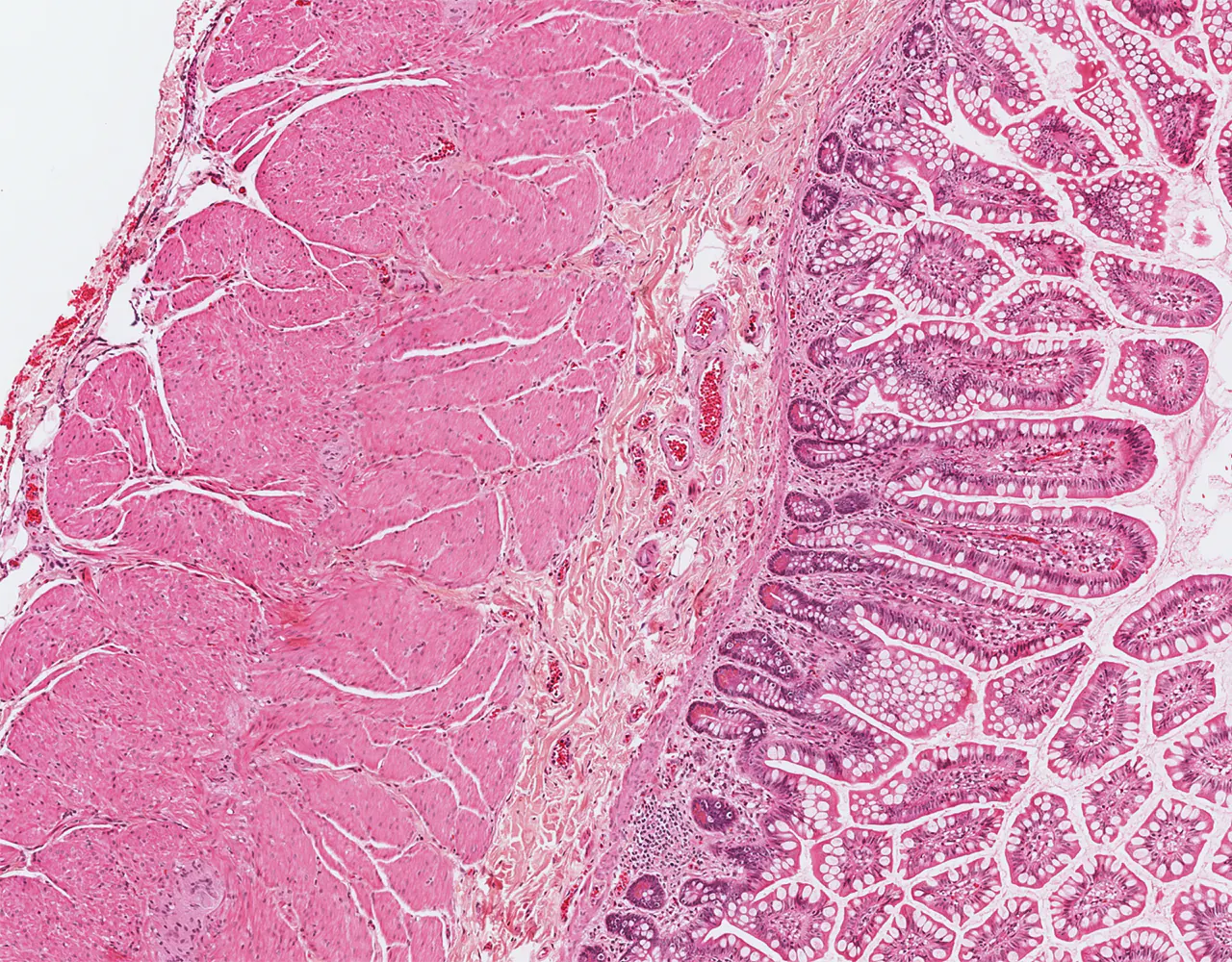



-p-130x130q80.png)

.webp)
.webp)