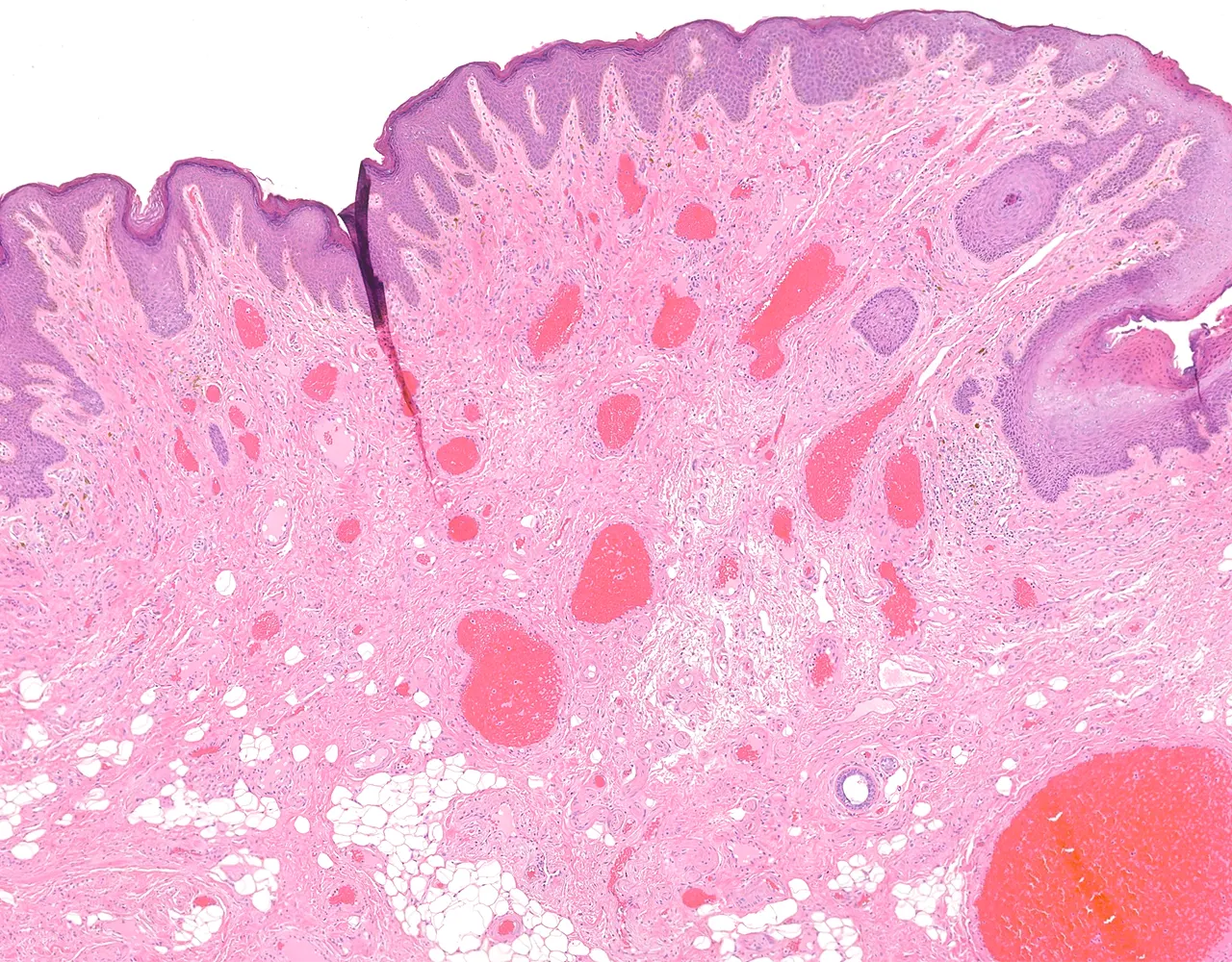
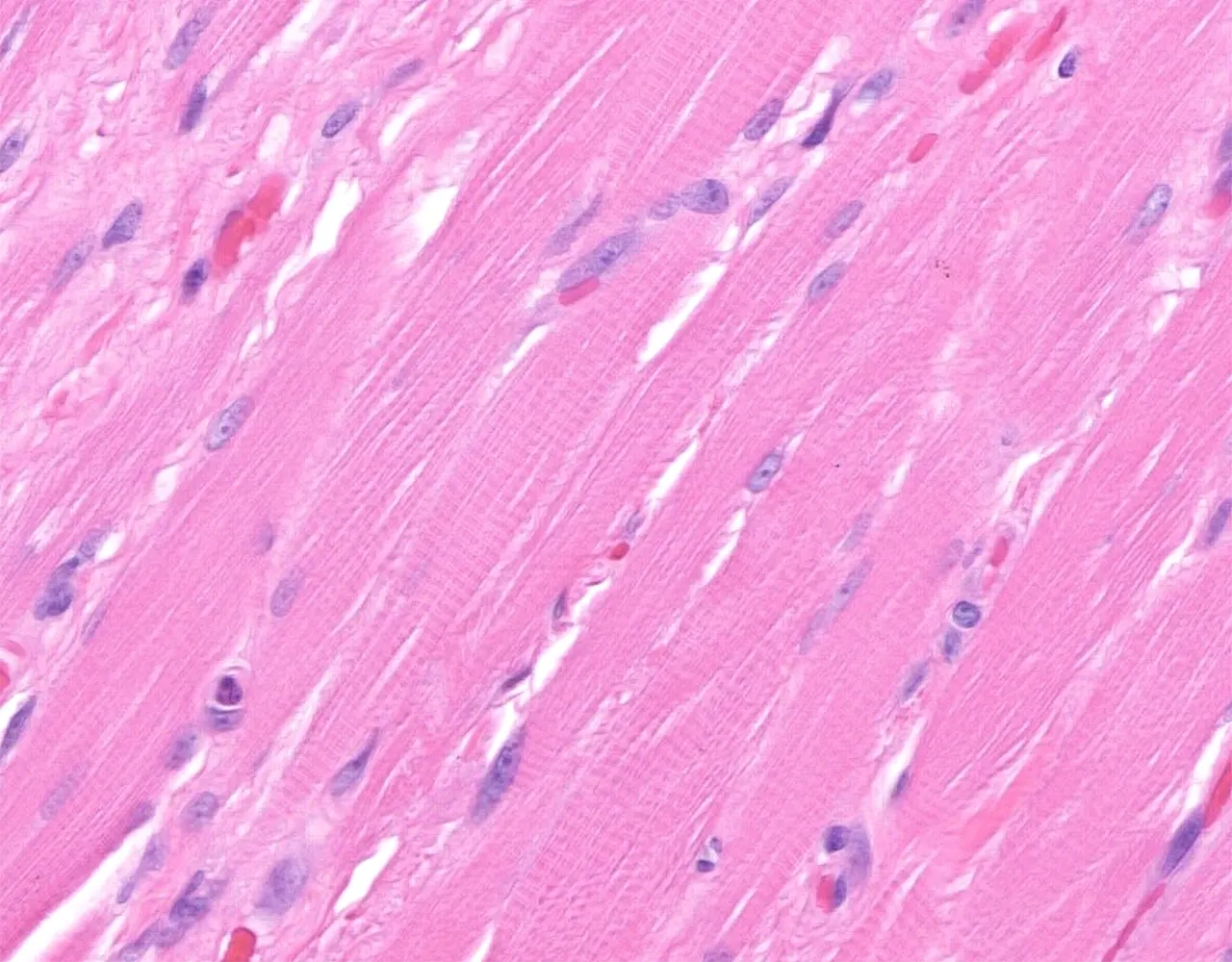
Overview
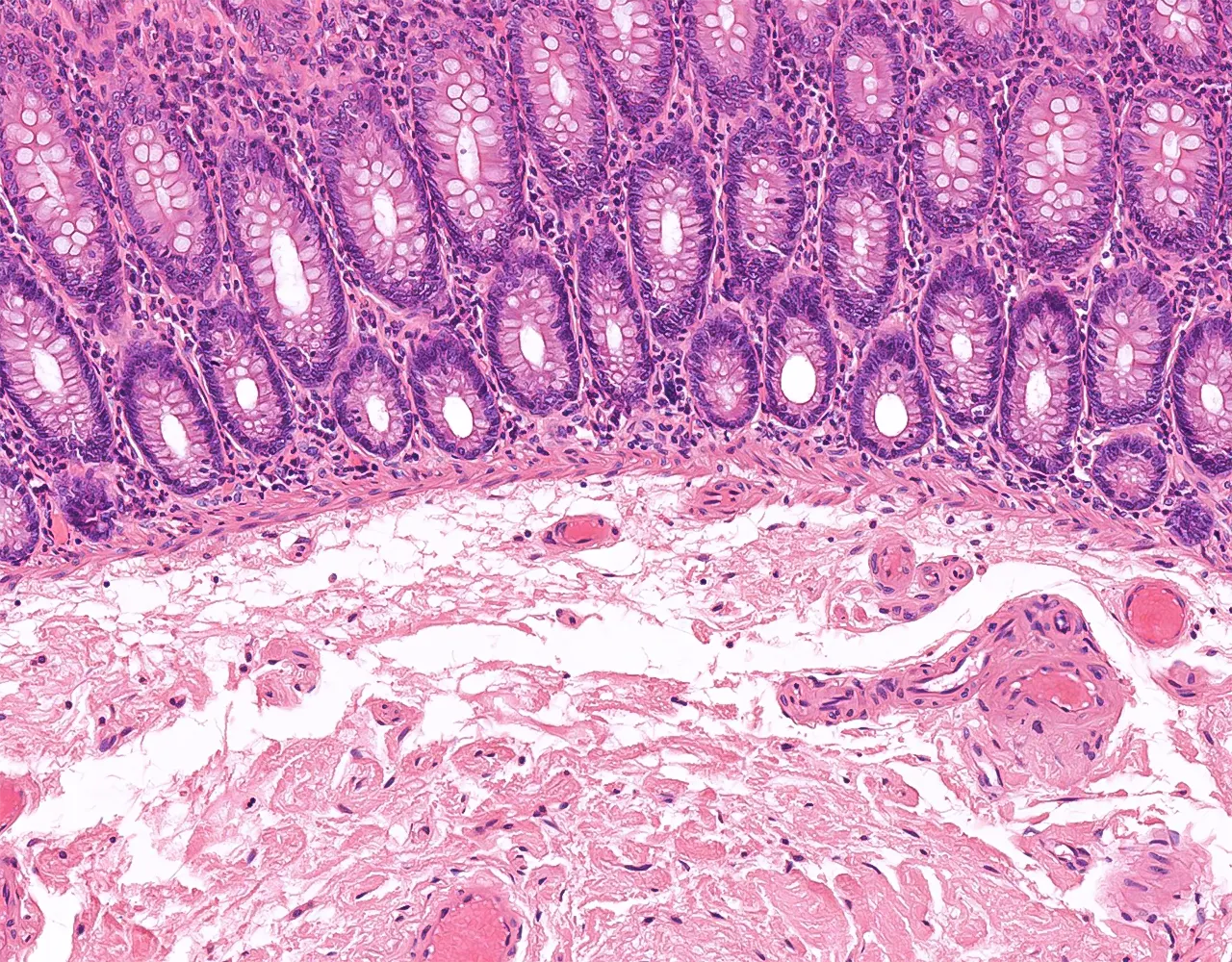
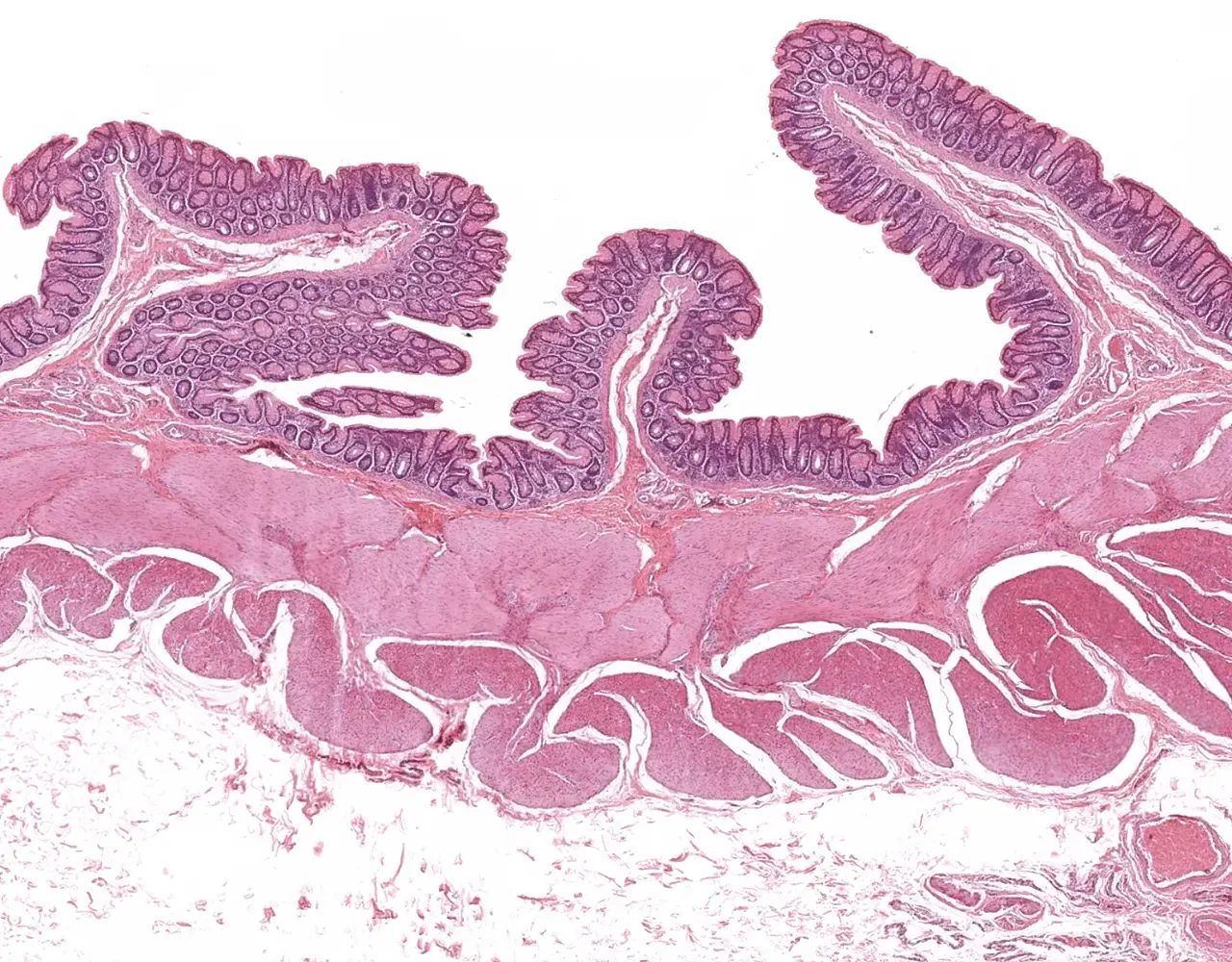
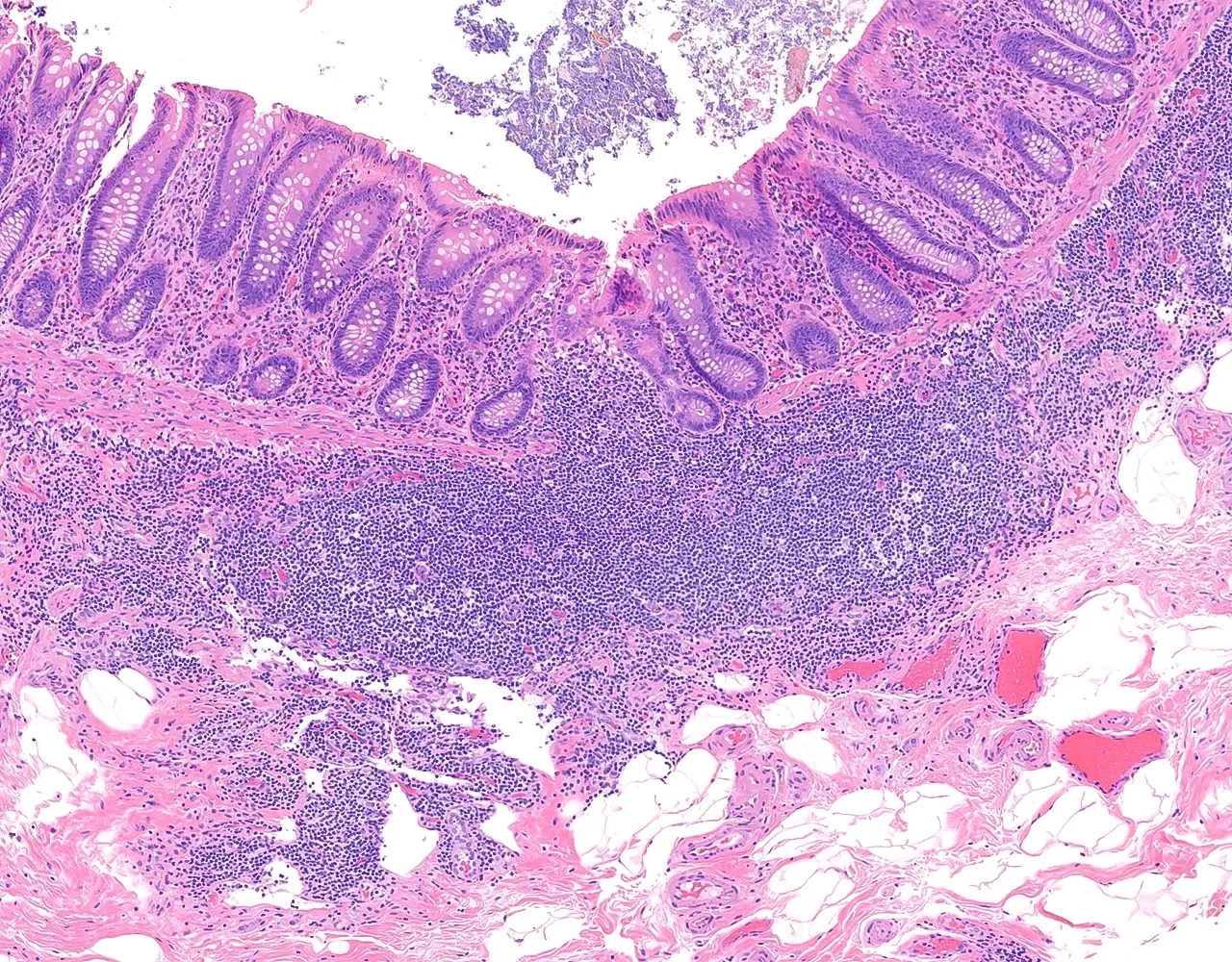
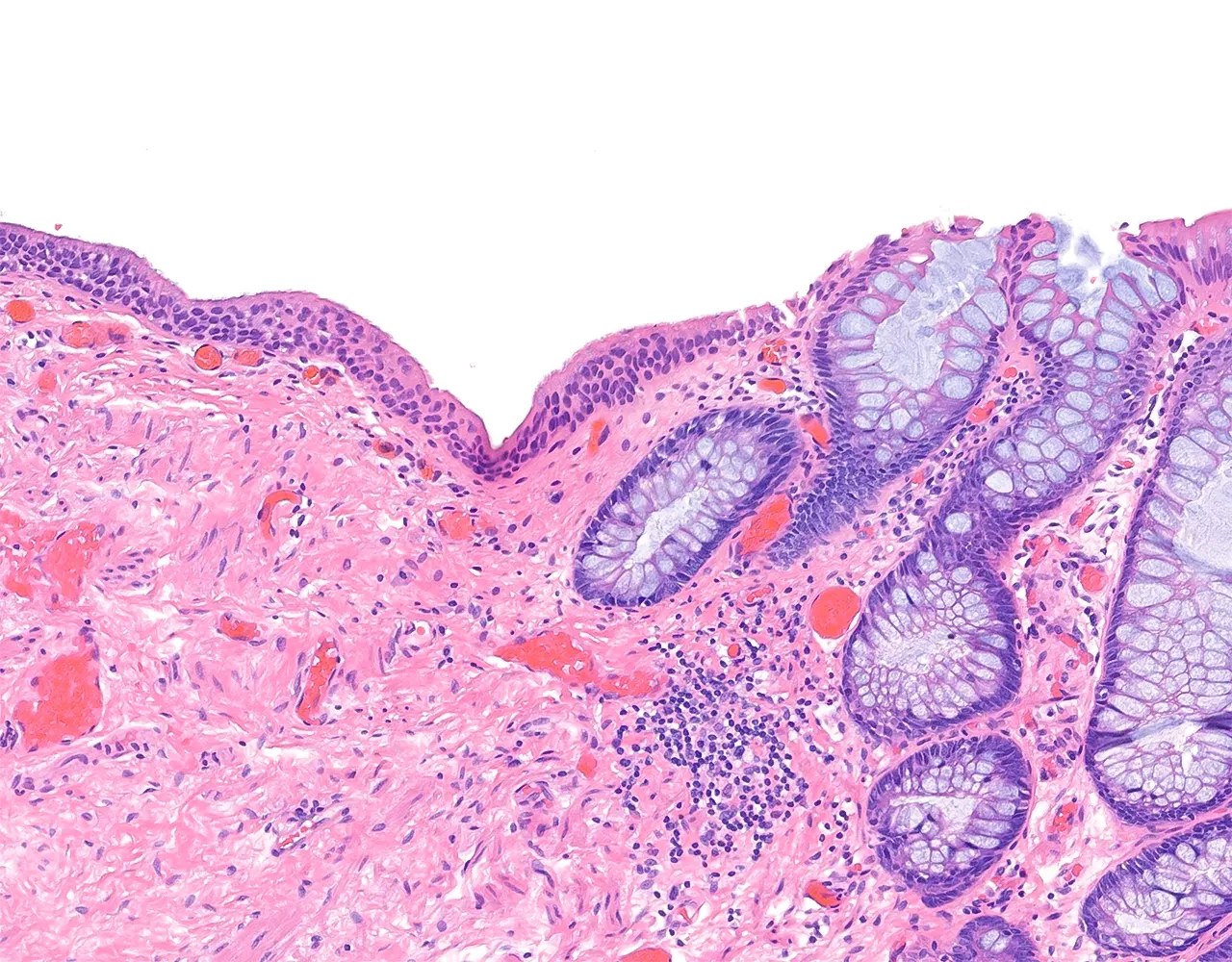
- The large intestine includes the cecum, colon, rectum, and anal canal.
- The right colon comprises the ileocecal valve, cecum, ascending colon, hepatic flexure, and proximal transverse colon.
- The left colon comprises the distal transverse colon, splenic flexure, descending colon, sigmoid colon, and rectum.
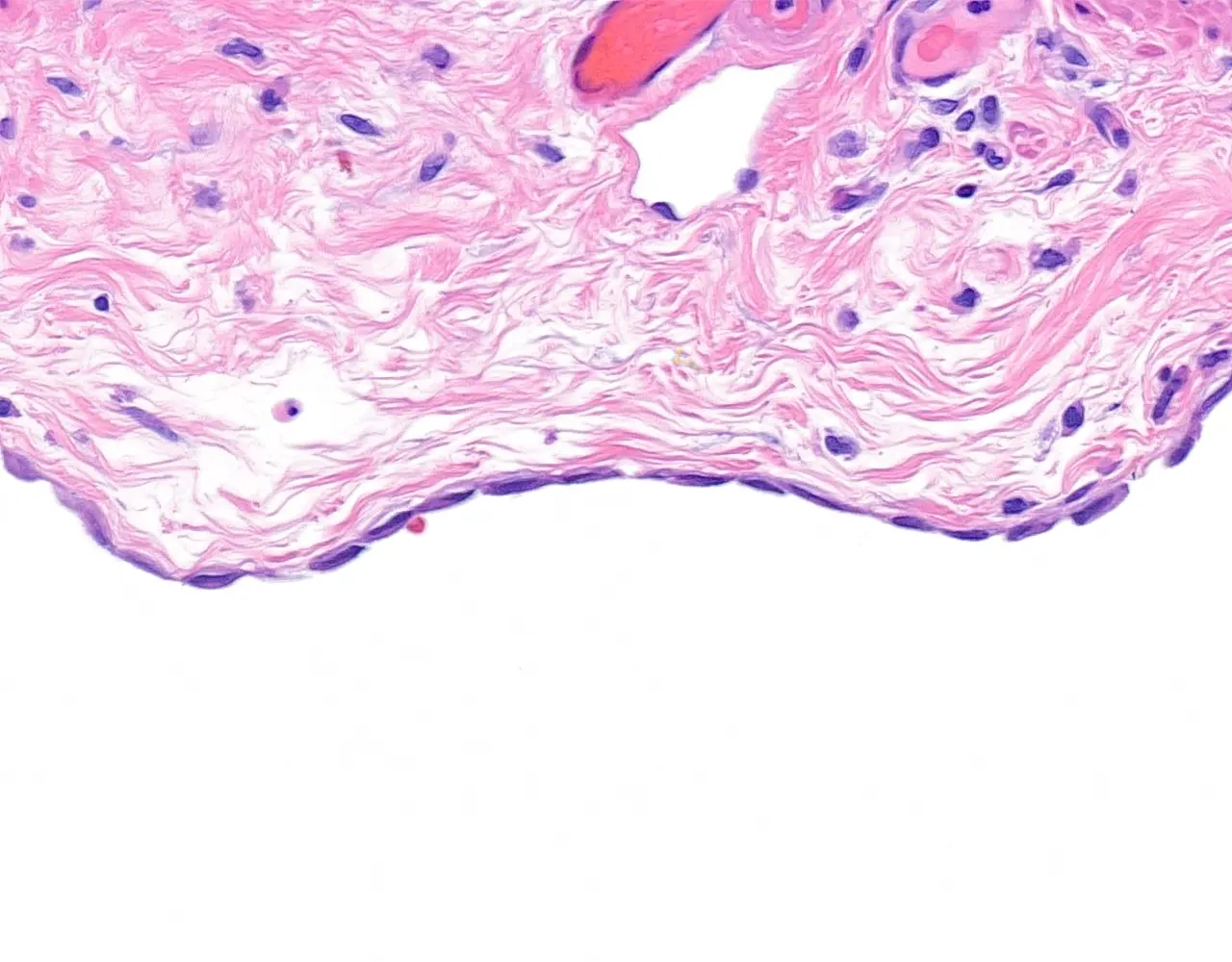
- The ascending and descending colon are mostly retroperitoneal, whereas the transverse and sigmoid colon are intraperitoneal and covered by serosa.
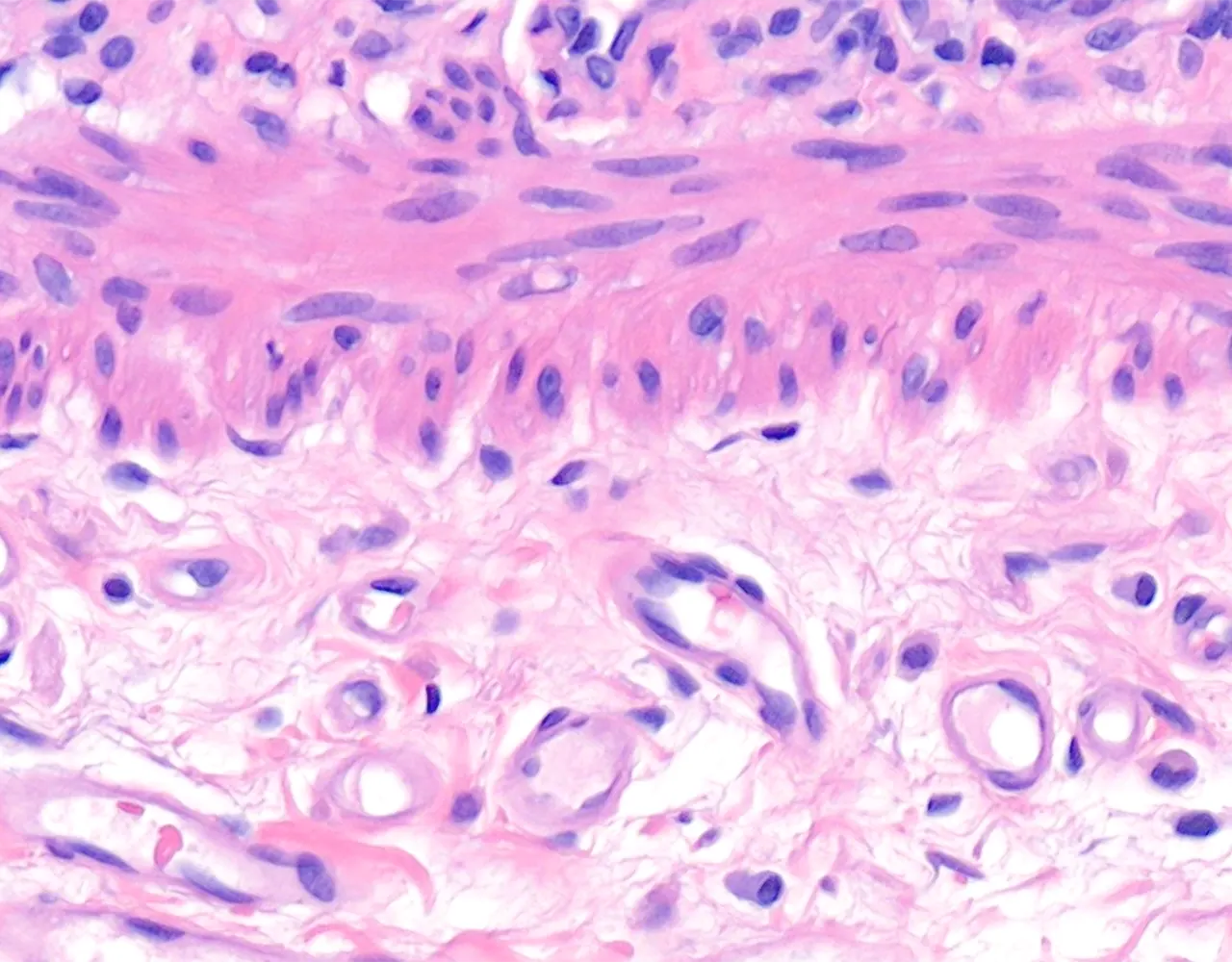
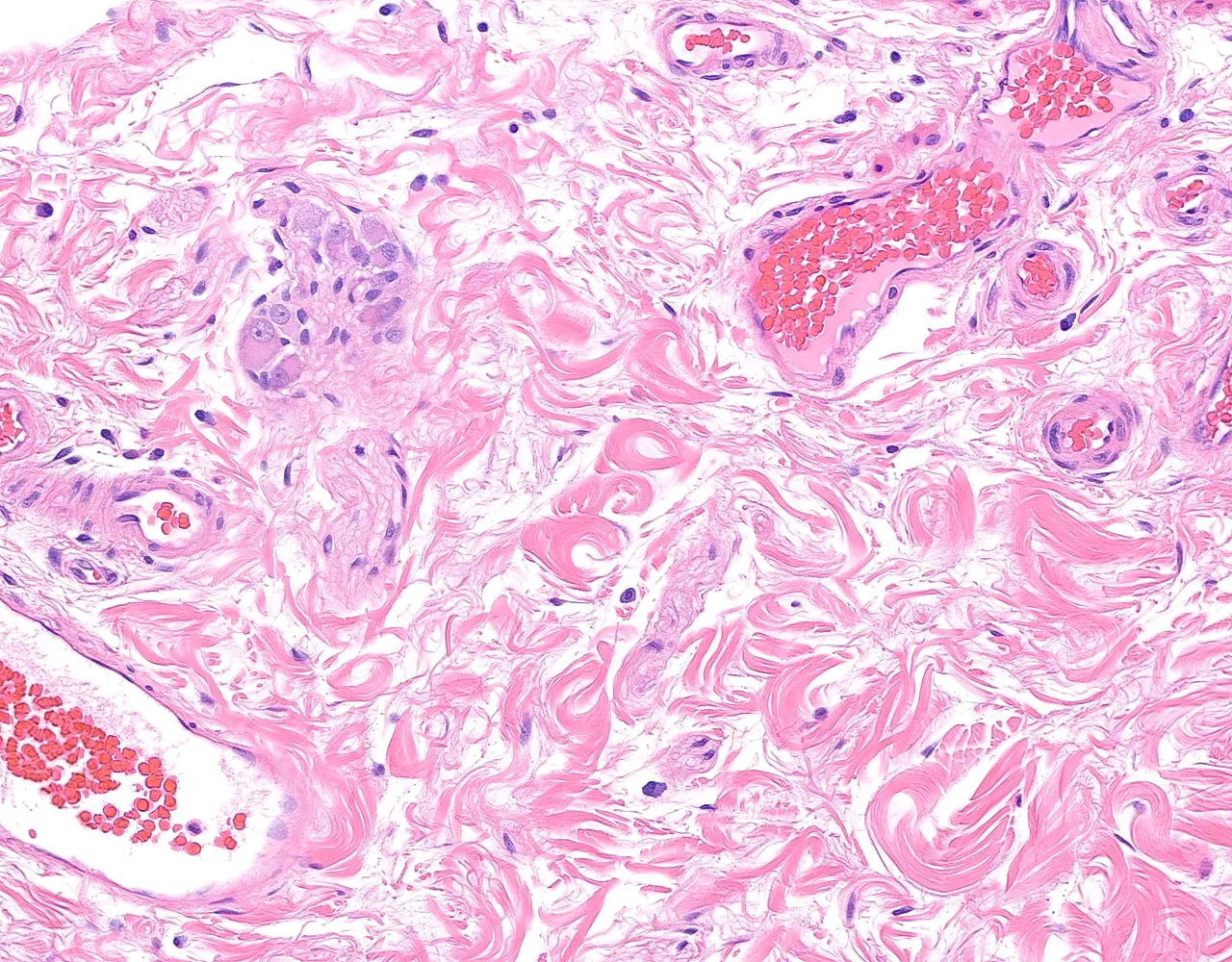
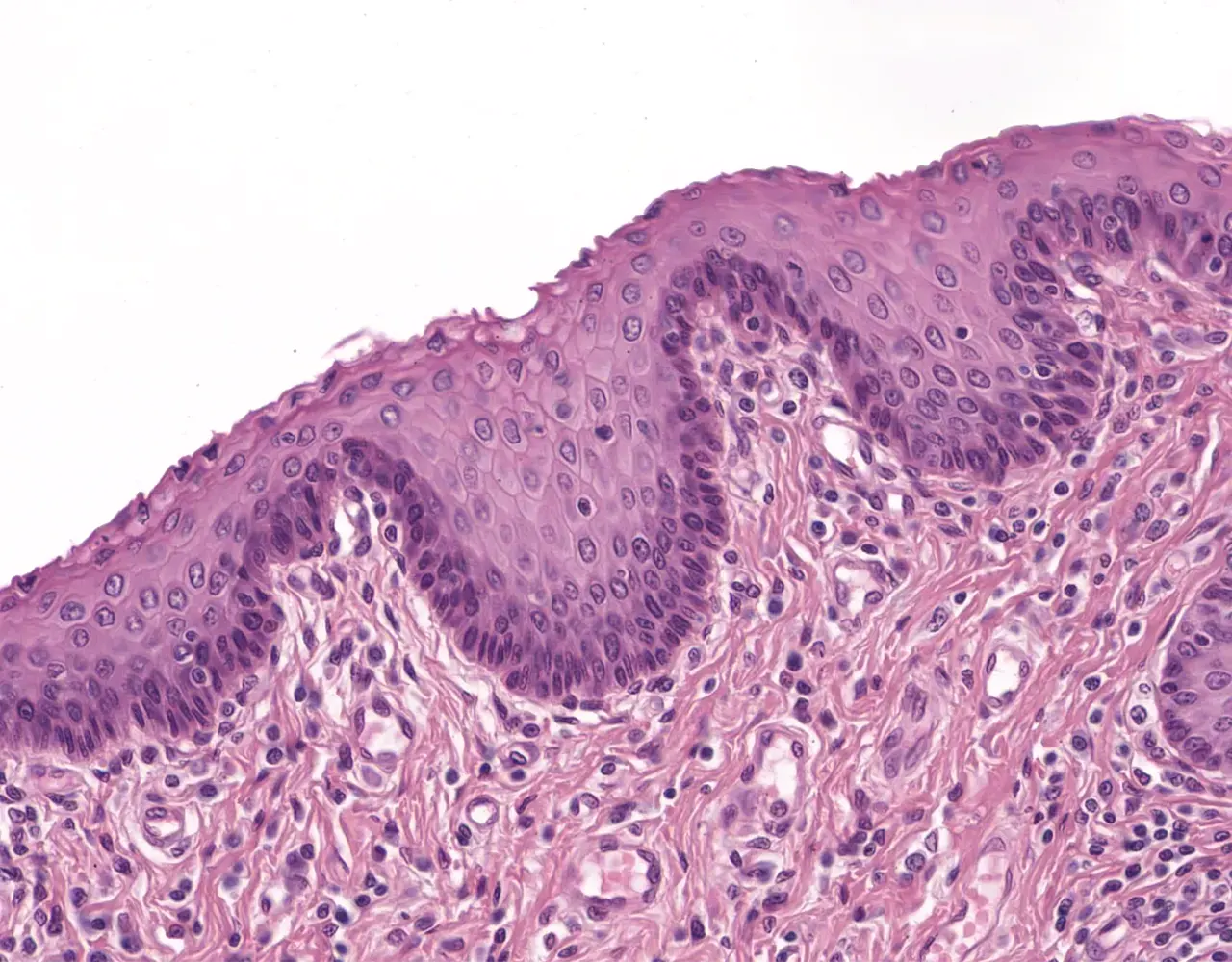
- The rectum is only partially covered by serosa proximally and is otherwise surrounded by adventitia.
- Functions :
- The large intestine is responsible for absorption of water and electrolytes, secretion of mucus for lubrication, compaction and storage of fecal material, and contribution to host-microbiota interactions.
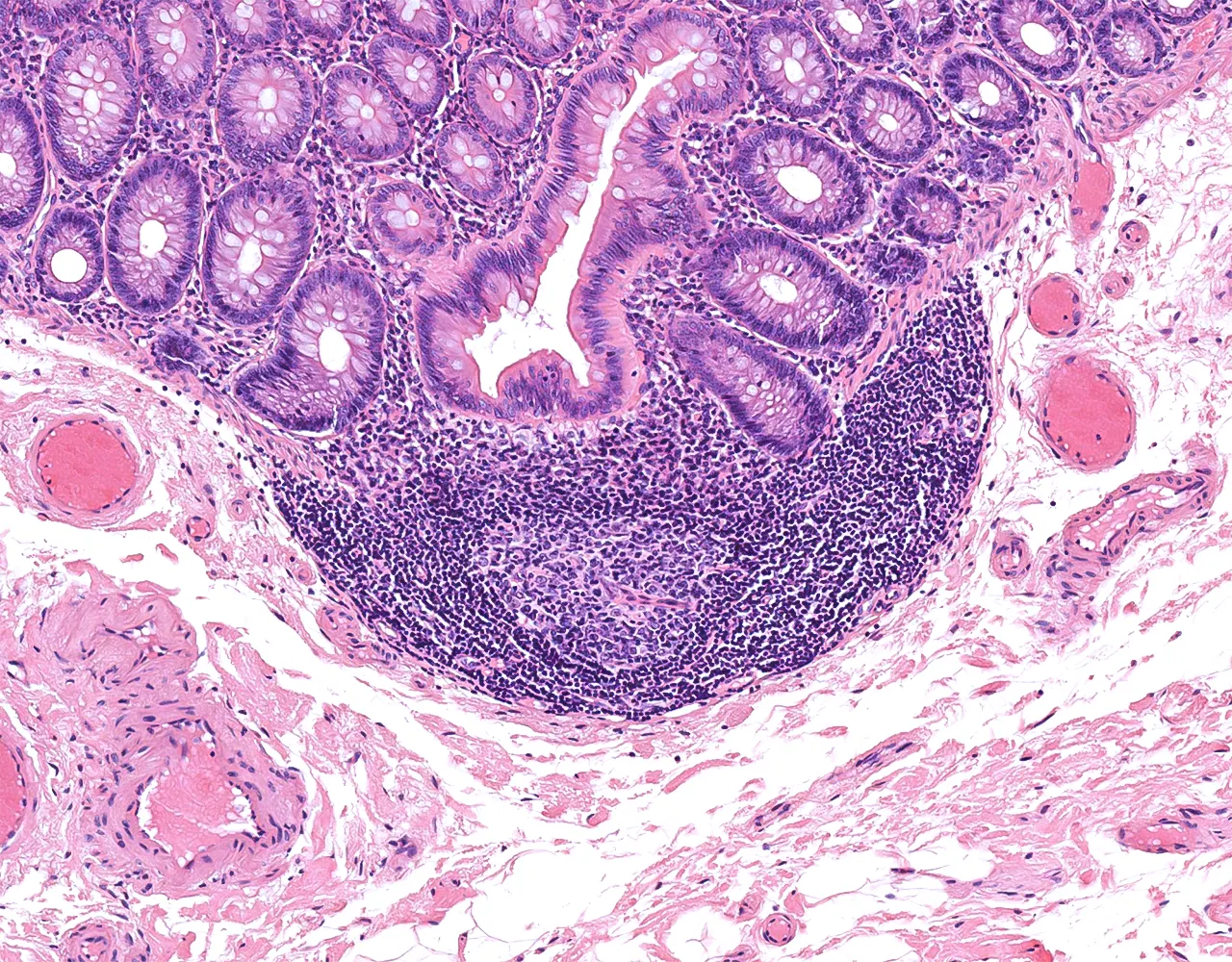
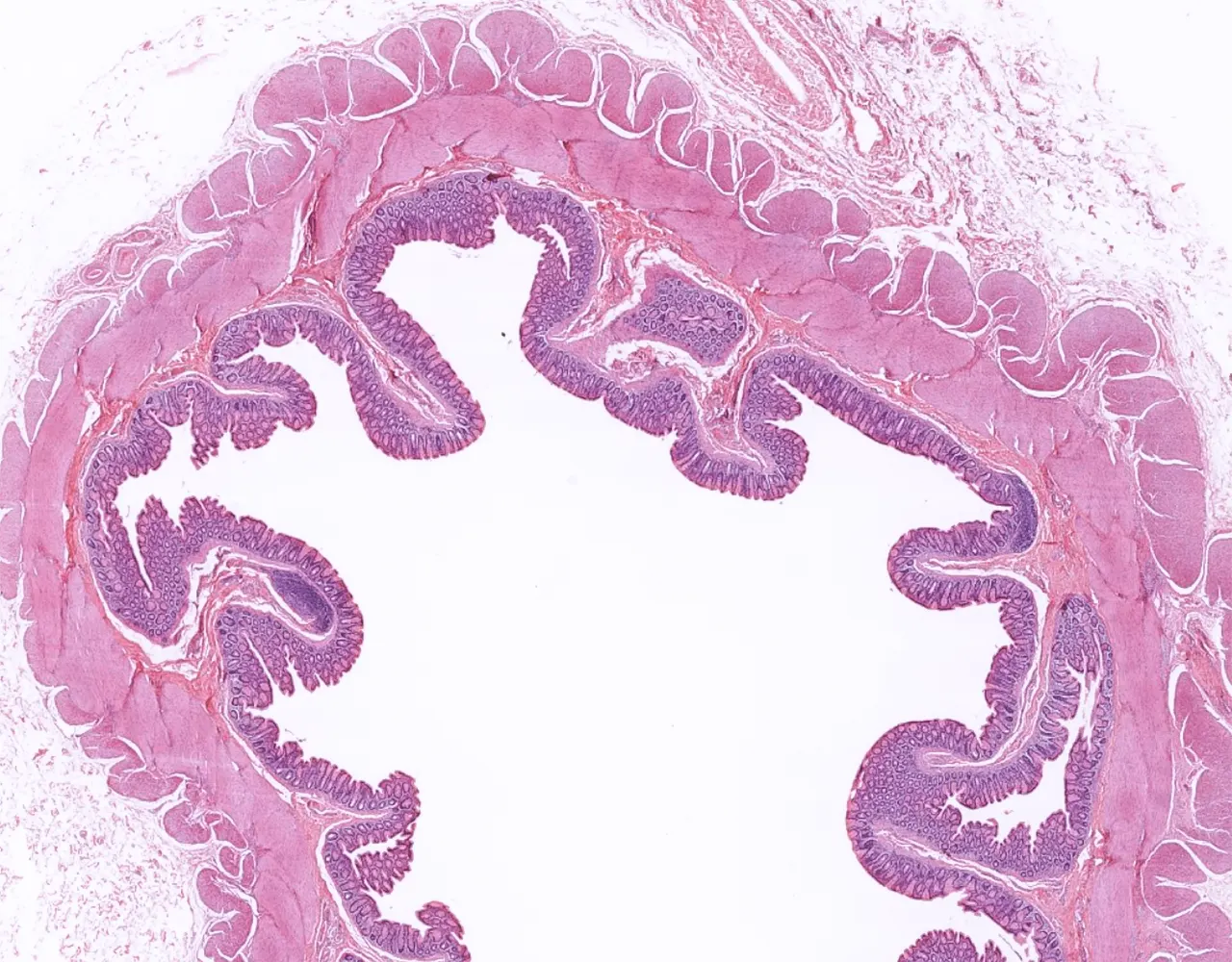
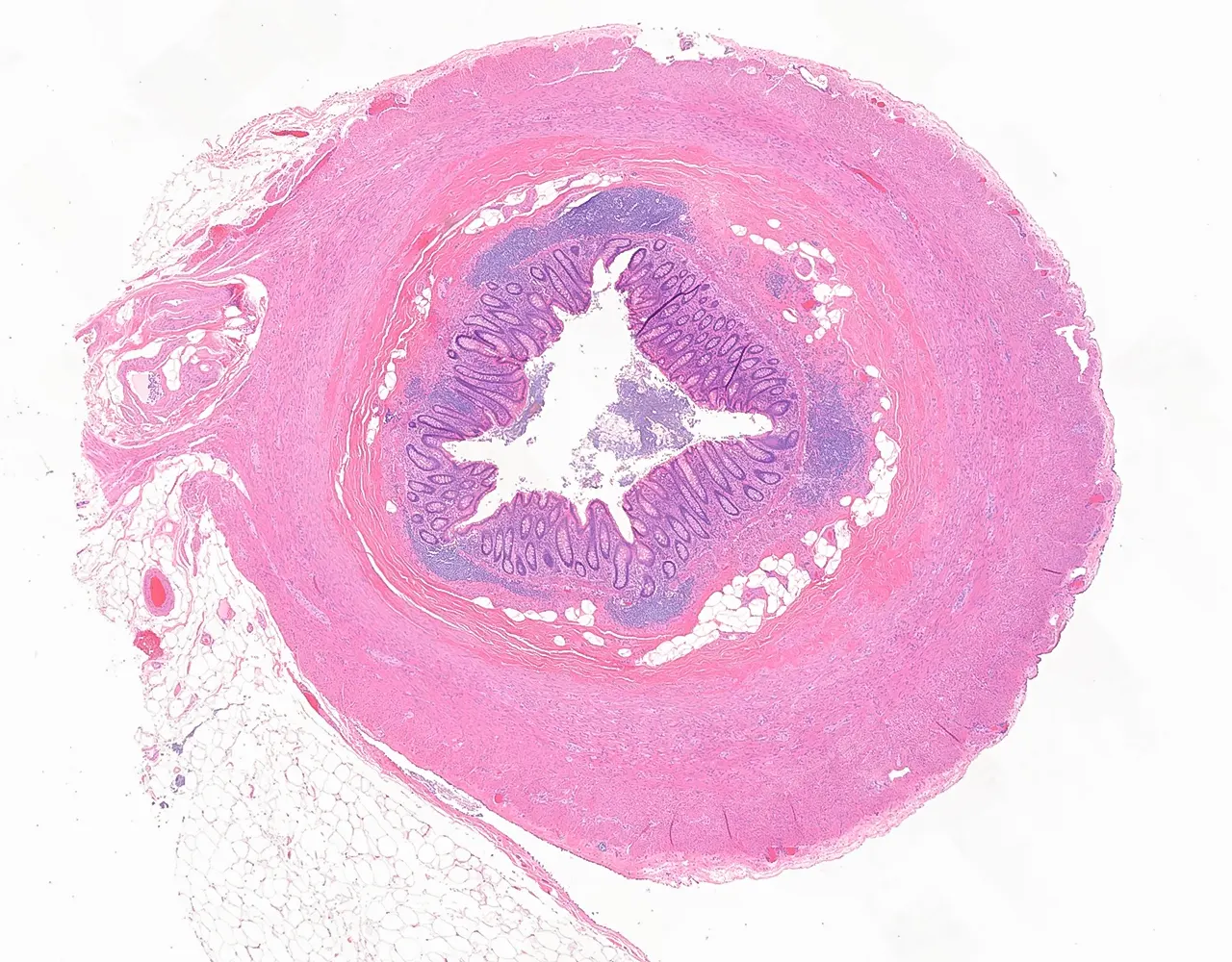
- The appendix is a blind diverticulum arising from the cecum :
- It contributes mainly to local immune function through its abundant lymphoid tissue and may also act as a reservoir for normal intestinal microbiota.

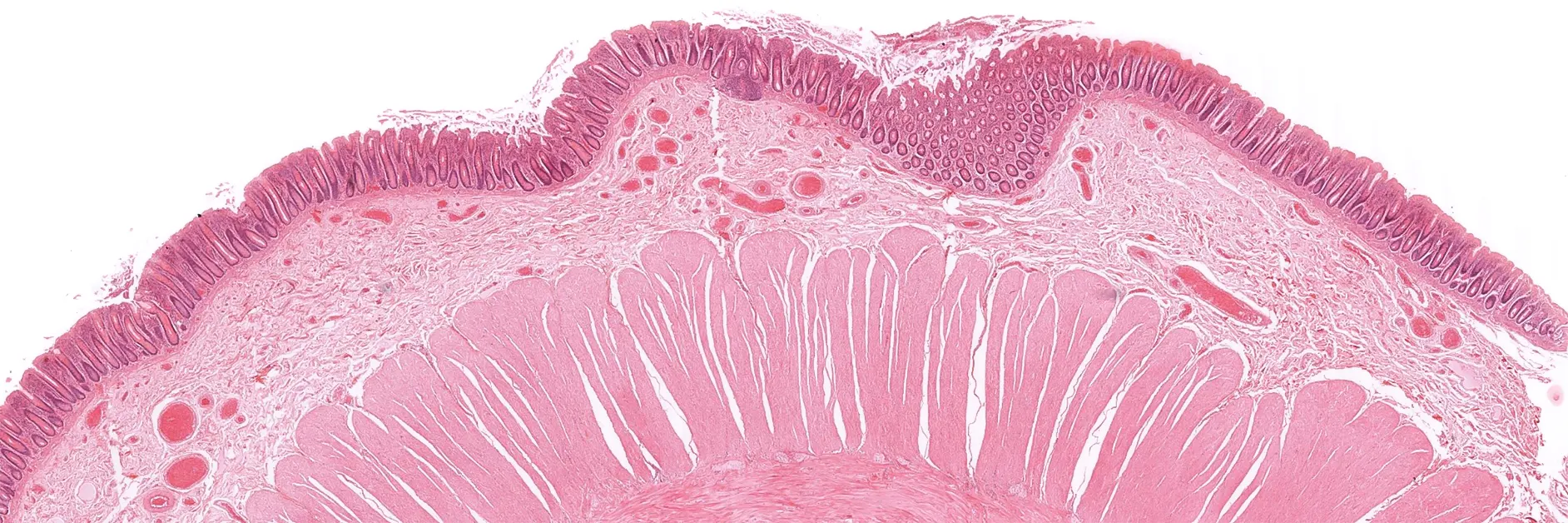
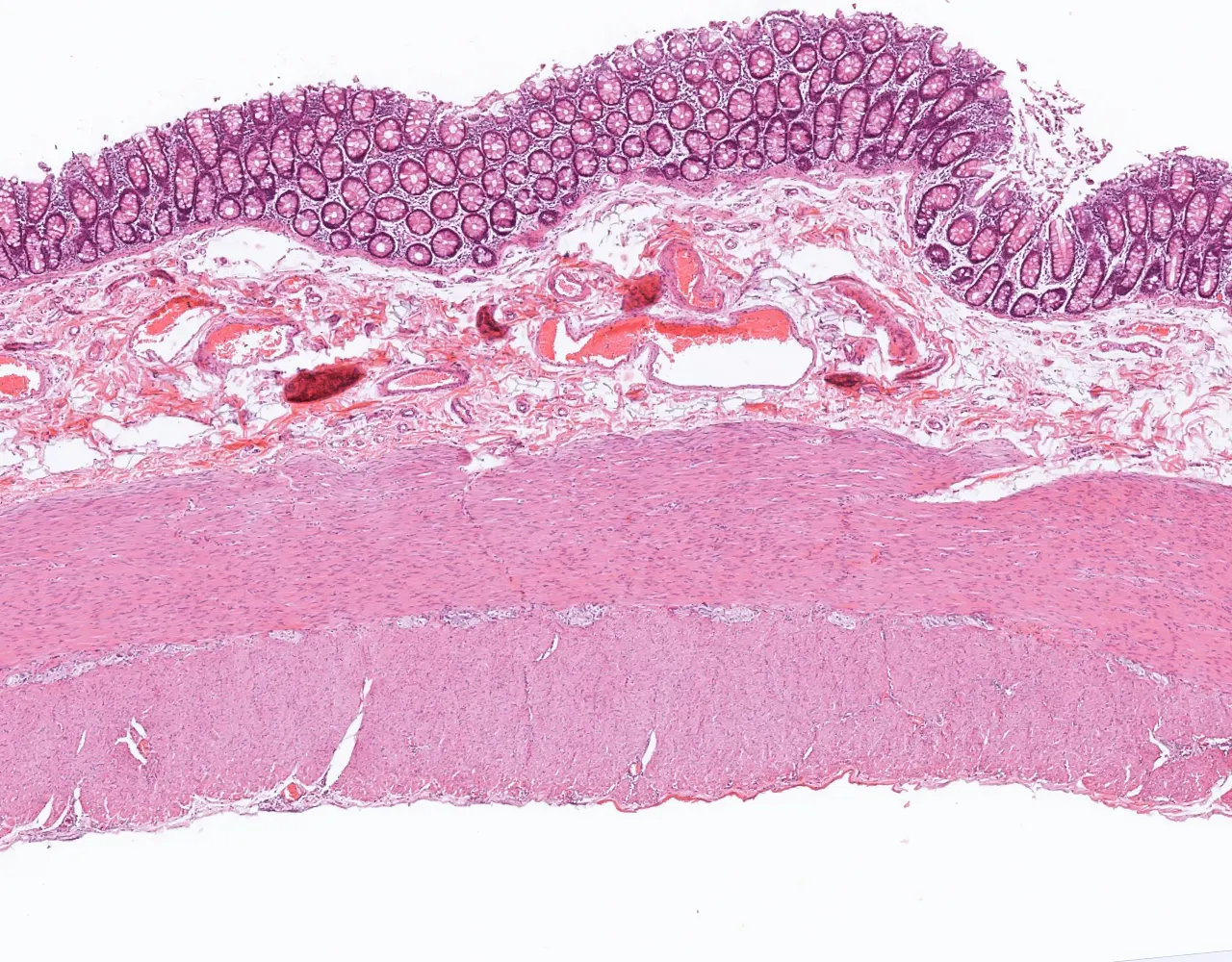


.webp)



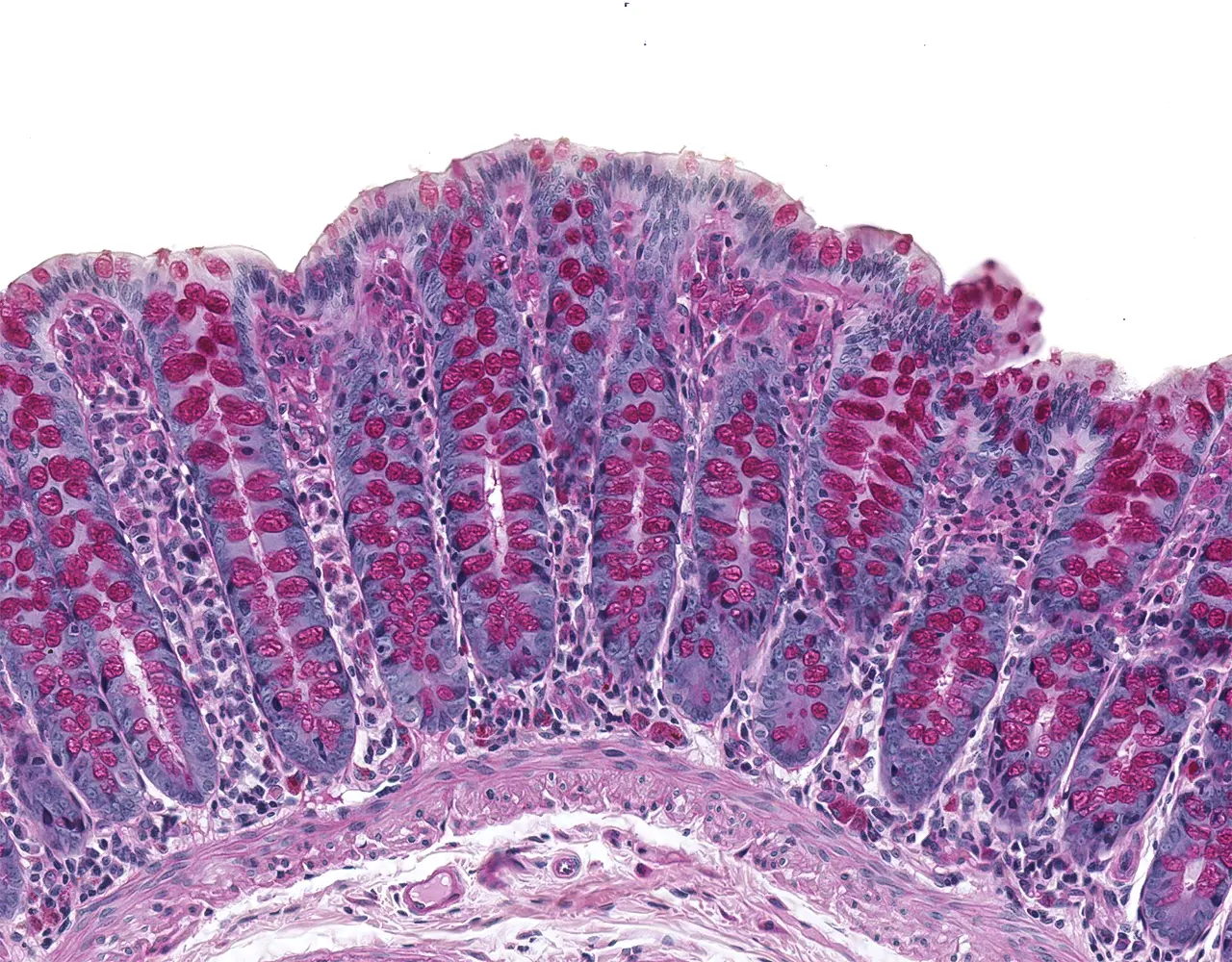
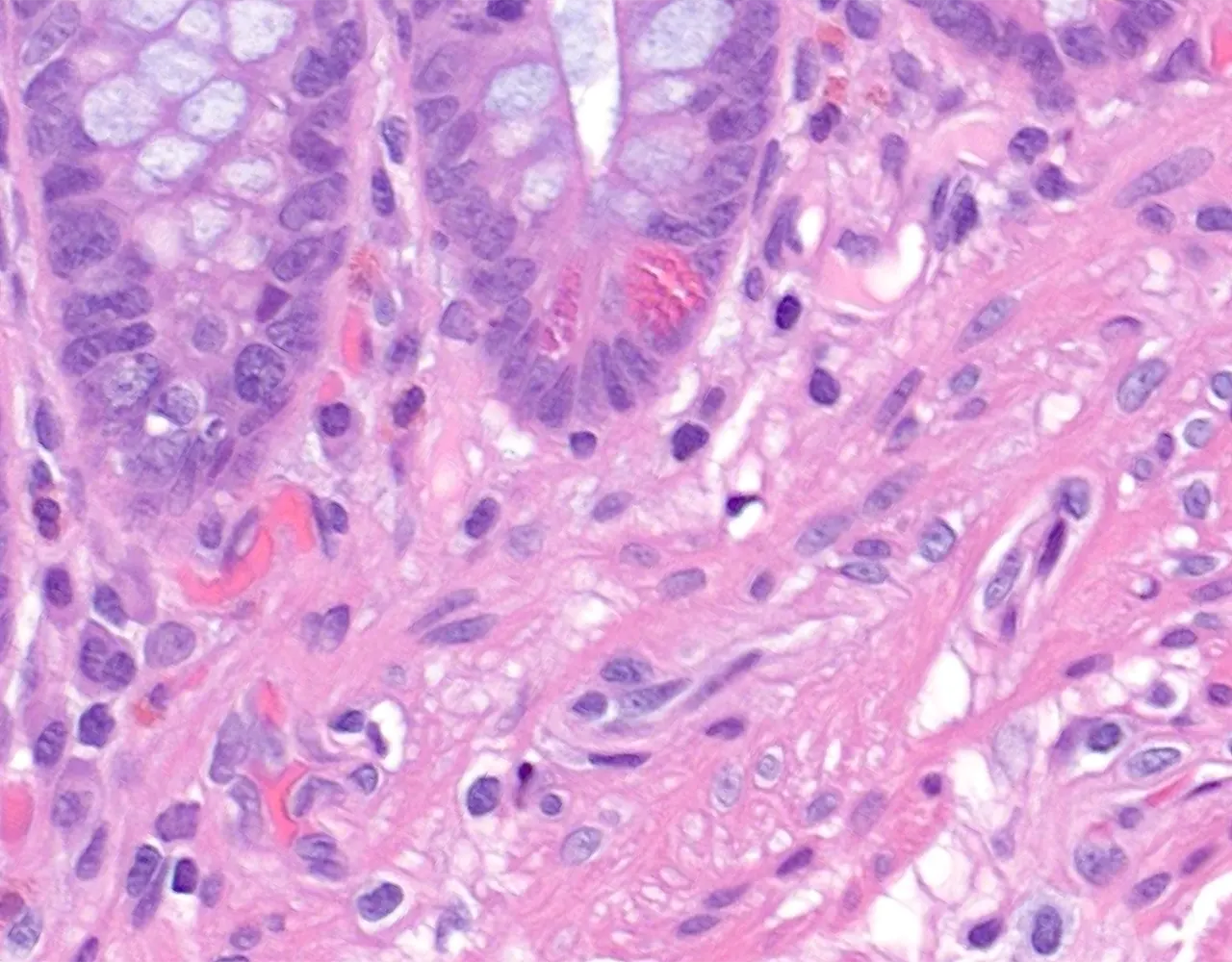

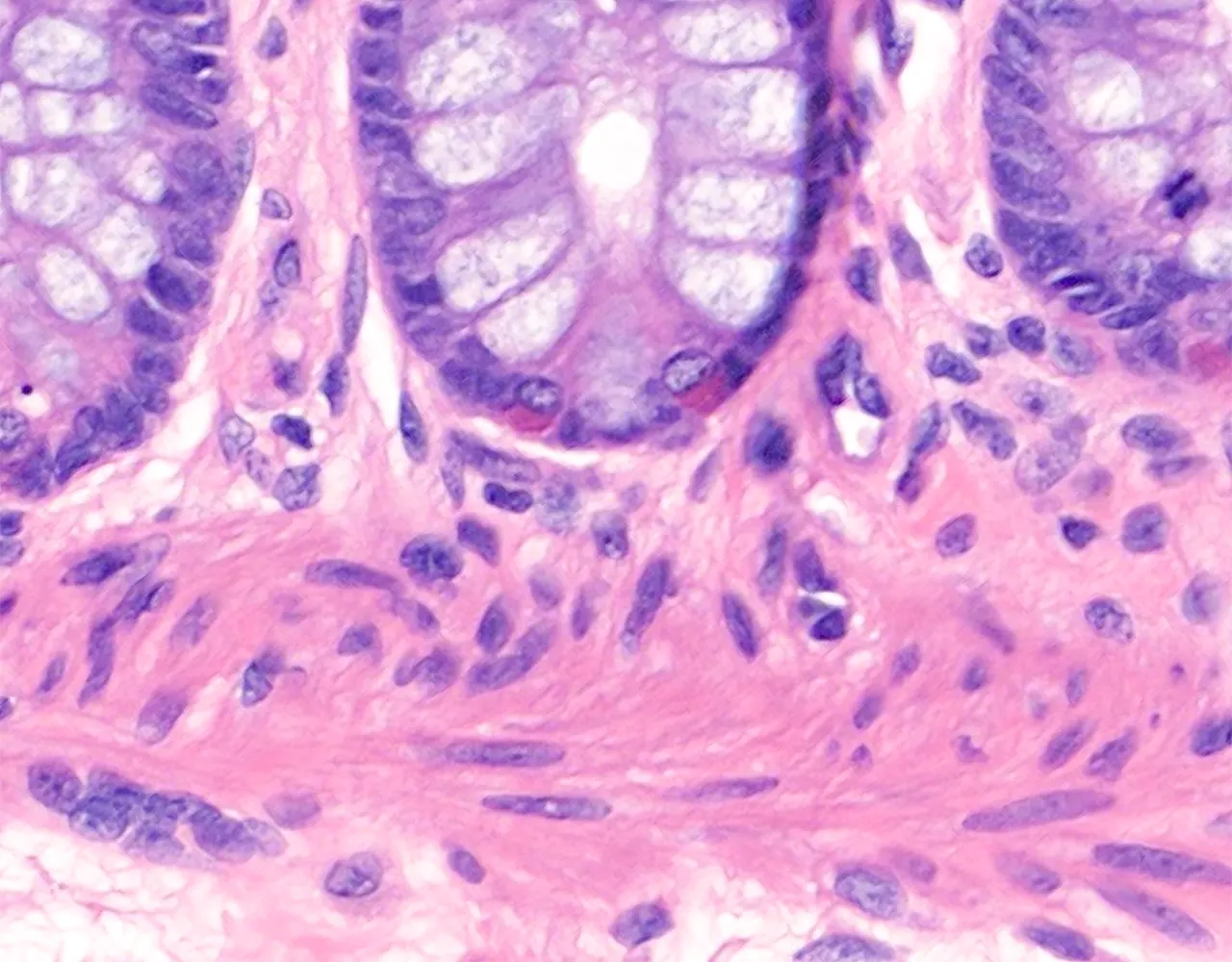
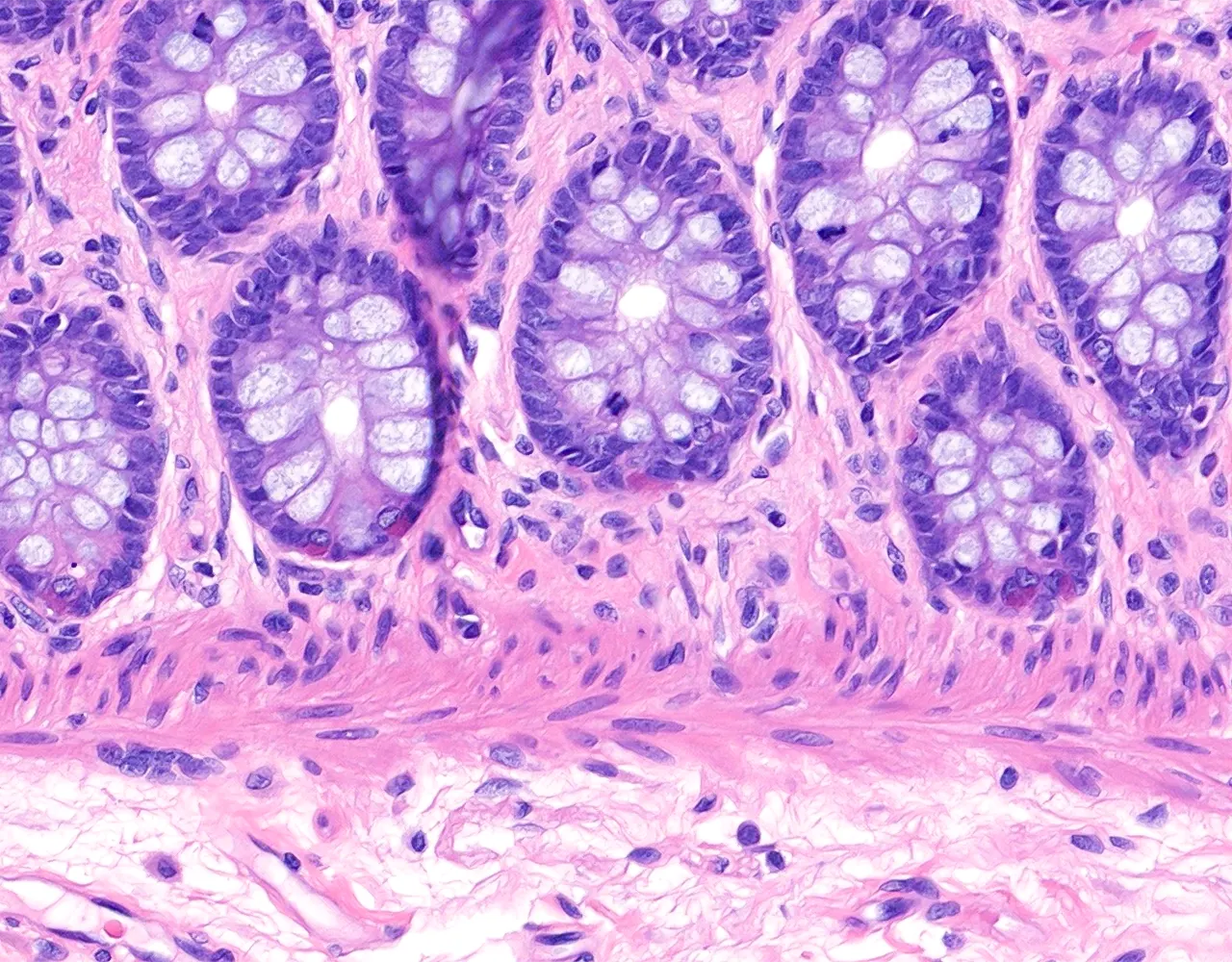
-p-130x130q80.png)
.webp)